You are here
- Home
- Publications and reports
- Data insights
- Health professionals: skills opportunities and challenges (2023 update)
Health professionals: skills opportunities and challenges (2023 update)
Summary
In 2022, health professionals accounted for around 3 per cent of all employment in the EU. These workers have been at the forefront in coping with the recent Covid-19 pandemic and are important in facilitating the living conditions of Europe’s ageing population. They study human and animal disorders, illnesses, and ways of treating them, and advise on or apply various measures to prevent and cure illnesses. Jobs within this group include general and specialised medical doctors, nurses, midwifes, paramedics, and veterinarians.
Key facts
- Around 6 million people were employed as health professionals in 2022, which accounts for 3 per cent of the total EU employment in that year.
- Between 2012 and 2022, health professionals’ employment increased by 22 per cent.
- Health professionals were central in coping with the Covid-19 pandemic. Their employment increased by 115 thousand workers between 2019 and 2020. Employment increased further in the following year, and by the end of 2022, employment was more than 200 thousand workers above its 2019 level.
- The vast majority of health professionals (86 per cent) have attained a qualification level of ISCED 5 or above in 2021, equivalent to the education level achieved after completing secondary/ post-secondary non-tertiary education. The qualification level of the occupation is not expected to change over the period to 2035.
- Health professionals are mainly women – 70 percent in 2021.
- By 2035 over 7 million people are projected to be working as health professionals. This represents an increase of 1 million jobs compared to 2022.
- Future demand for health professional skills will be affected by population aging, the increased prevalence of diseases associated with older people, the emergence of new diseases brought by the changing European climate, and digital technologies facilitating health professionals’ work.
Employment and job demand
Employment growth of health professionals was slower than that of all professionals in the first years of the past decade. However, the growth has picked up significantly in 2018 and 2019, which is why in year-to-year comparison, the significant employment growth during the Covid-19 pandemic meant a slowing of the dynamic.
Figure 1: Year-to-year employment change for health professionals (2013-2022)
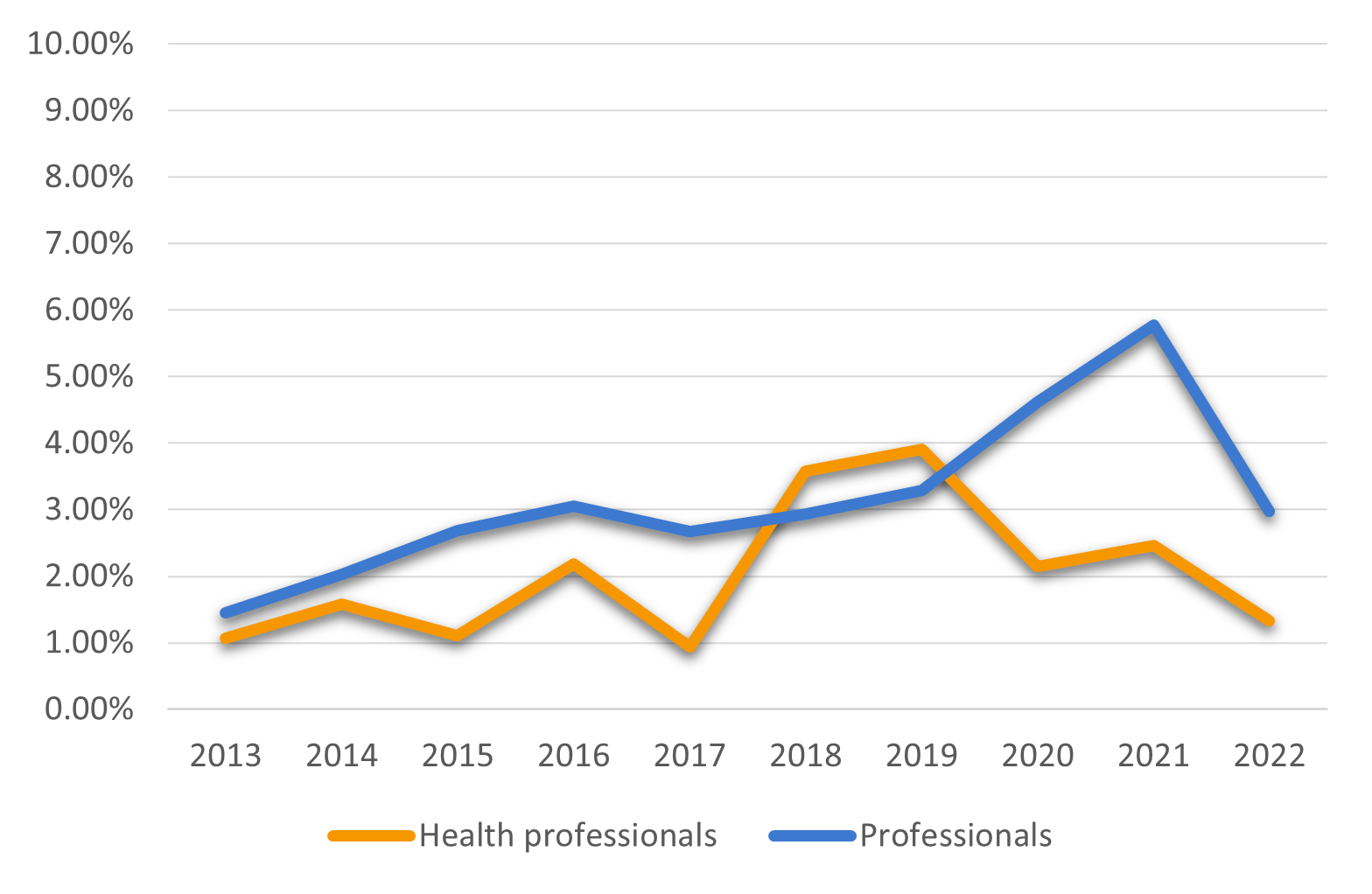
Source: European Labour Force Survey. Employed persons by detailed occupation (ISCO-08 two-digit level) [LFSA_EGAI2D__custom_7778289]. Own calculations.
More than a third of health professionals (35 per cent) are engaged as other health professionals. This group includes specialised professionals such as dentists, optometrists, speech therapists, dieticians, and occupational health and hygiene professionals.
About one third (32 per cent) are engaged as medical doctors (physicians) and another 30 per cent are engaged as nursing and midwifery professionals.
The rest of the health professionals are engaged as veterinarians, traditional and complementary medicine professionals, and paramedical practitioners.
Over time, the share of employment of these groups has changed only a little (see Figure 2).
Figure 2: Employment in health professionals’ jobs (in %)
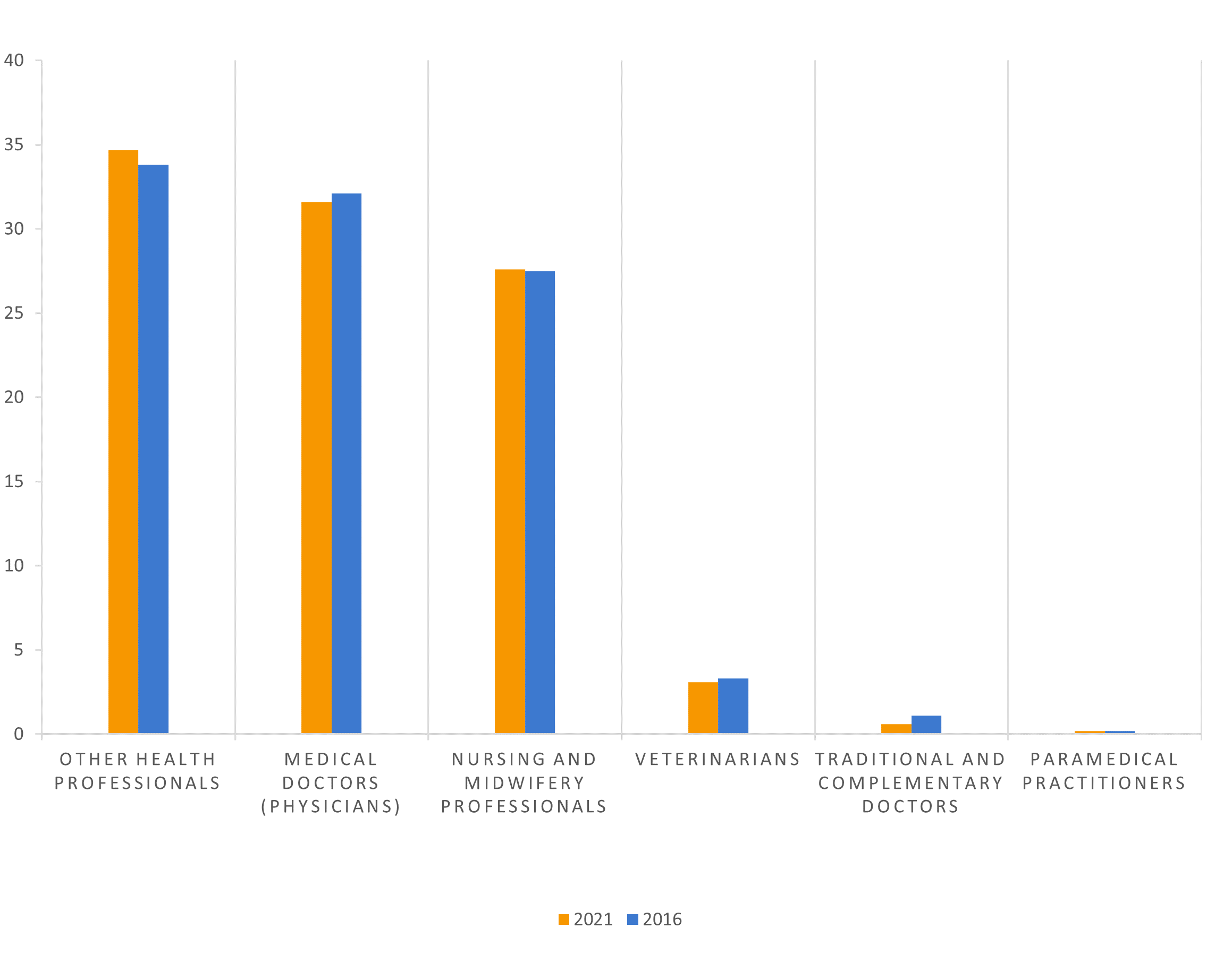
Source: European Labour Force Survey. Microdata. Own calculations.
The vast majority of OJAs for medical professionals tracked by the Cedefop system comprise of only three sub-categories: medical doctors, other health professionals and nursing professionals (these three occupations also constitute more than 90 per cent of the health professionals employment). There was a notable spike in demand for health professionals in OJAs in recent years. However, OJAs may not cover the existing job vacancies for these professionals fully, as these are often promoted via specialised channels.
For more details on skills demand and job openings for this occupation, please access the Cedefop’s Skills OVATE tool.
Figure 3: Online job advertisements for health professionals (2022, in %)
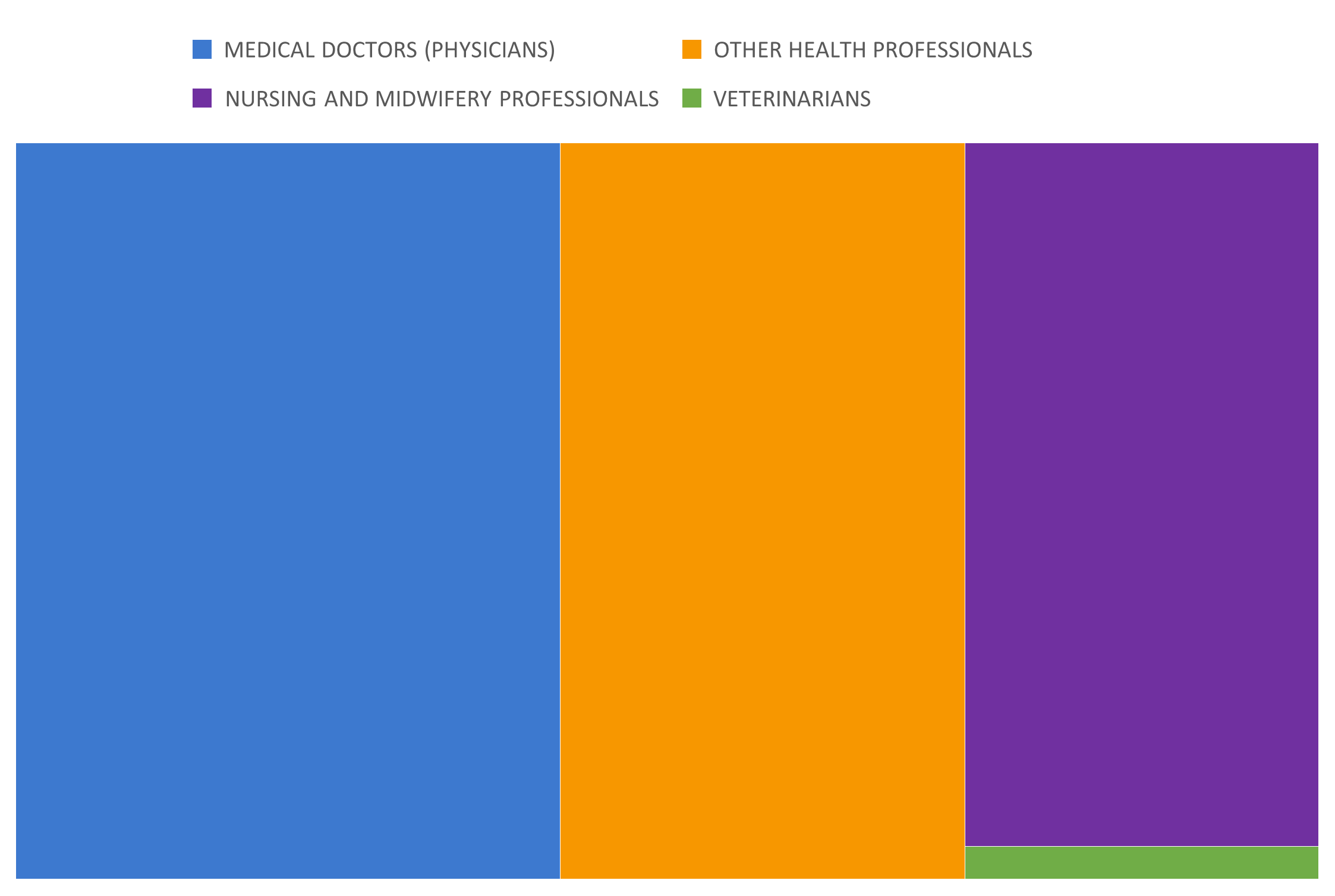
Source: Skills in Online Job Advertisements indicator based on Cedefop’s Skills OVATE. Own calculations. Note: Online job advertisements are by definition not equivalent to job vacancies. See Beręsewicz (2021) or Napierala et al. (2022).
The health sector employs the majority of health professionals. The wholesale and retail trade sector is the only other sector with a significant number of health professionals, accounting for 8 per cent of their employment. This concerns mainly workers in pharmacies.
Figure 4: The top sectors employing health professionals (in %)
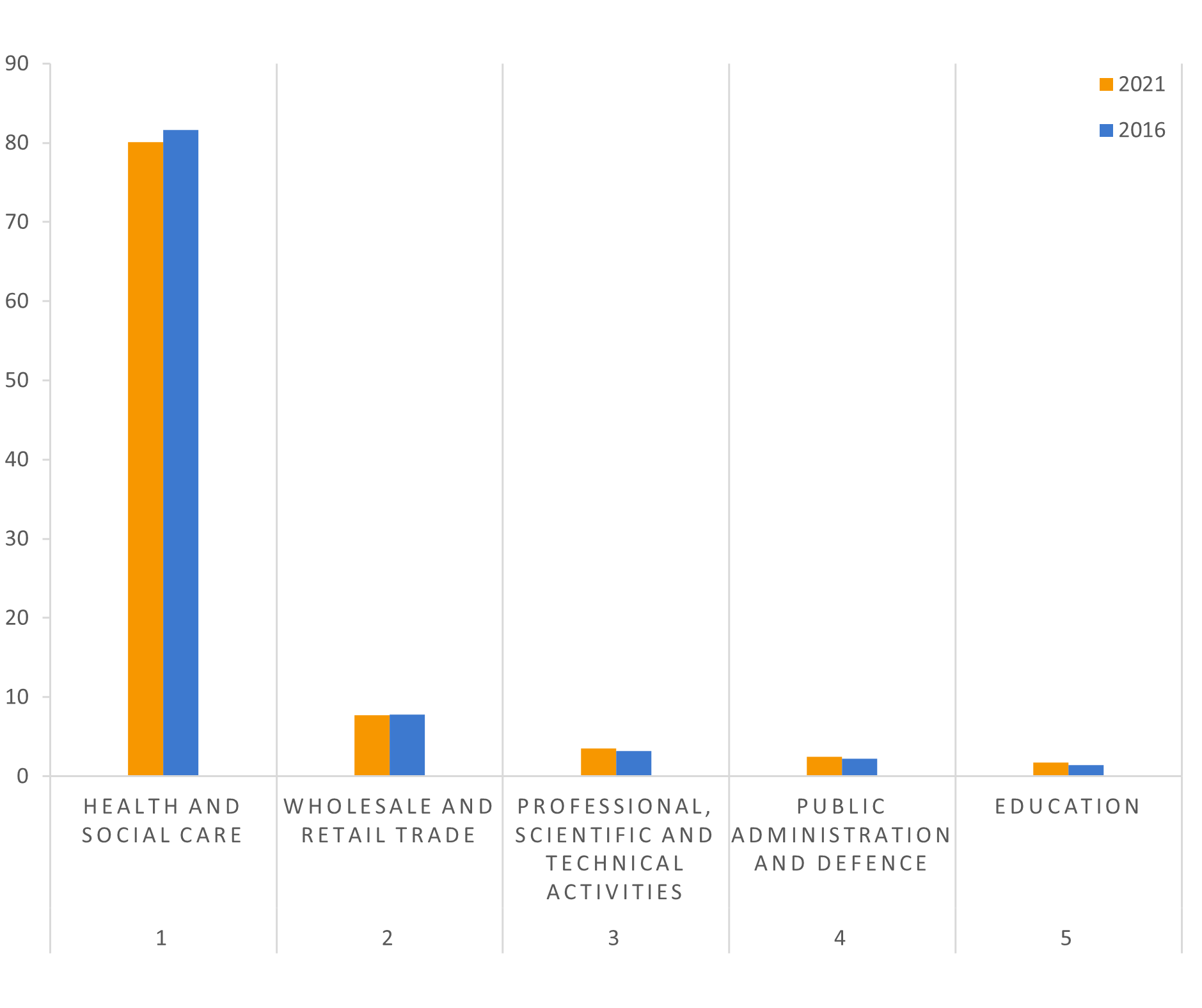
Source: European Labour Force Survey. Microdata. Own calculations.
There are notable differences in the employment share of health professionals across countries. In some, especially in the north of Europe, but also in Austria, Portugal, Belgium, Netherlands or Greece – this share approaches or exceeds 5 per cent, while it remains much lower in others, including Hungary, Germany or Slovakia.
Figure 5: Health professionals as a share of country employment (2021, in %)
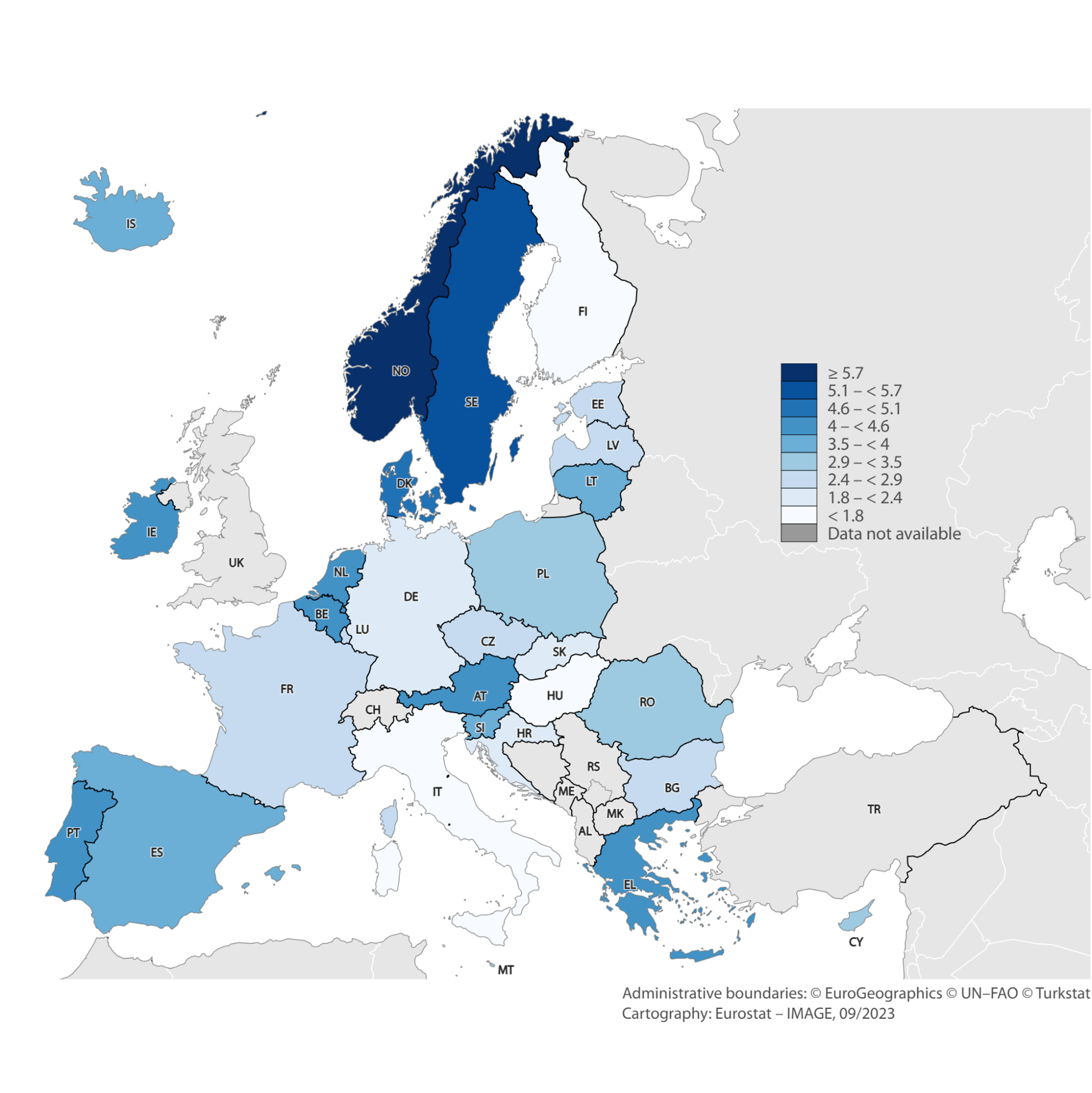
Source: European Labour Force Survey. Microdata. Own calculations.
Note: Data for CY, EE, IS, LV and LU have lower reliability because of the small sample size.
LFS data for MT are not available.
The workforce is composed of mainly women (70 per cent in 2021). While ageing remains an issue for the health professionals’ workforce, there is a steady inflow of younger talent, too. The employment share of workers younger than 50 years has slightly increased between the 2016-2021 period.
Figure 6: Health professionals by age (in %)
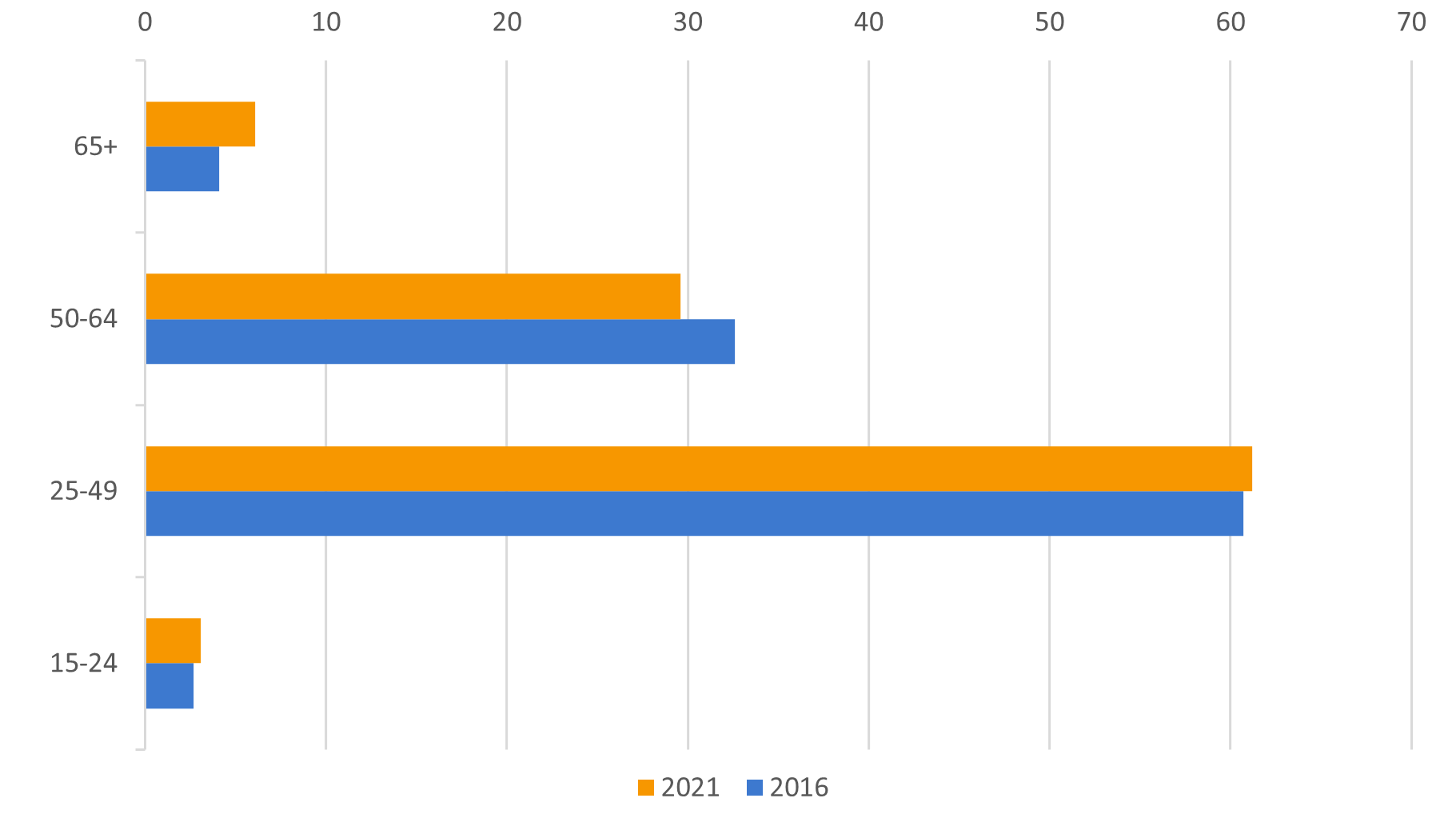
Source: European Labour Force Survey. Microdata. Own calculations.
Health professionals usually have lower job turnover than other occupations, meaning that on average they stay at one job for a longer time. They also tend to have a slightly higher share of part-time or temporary contracts.
Figure 7: Contract and hiring trends for health professionals (in %)
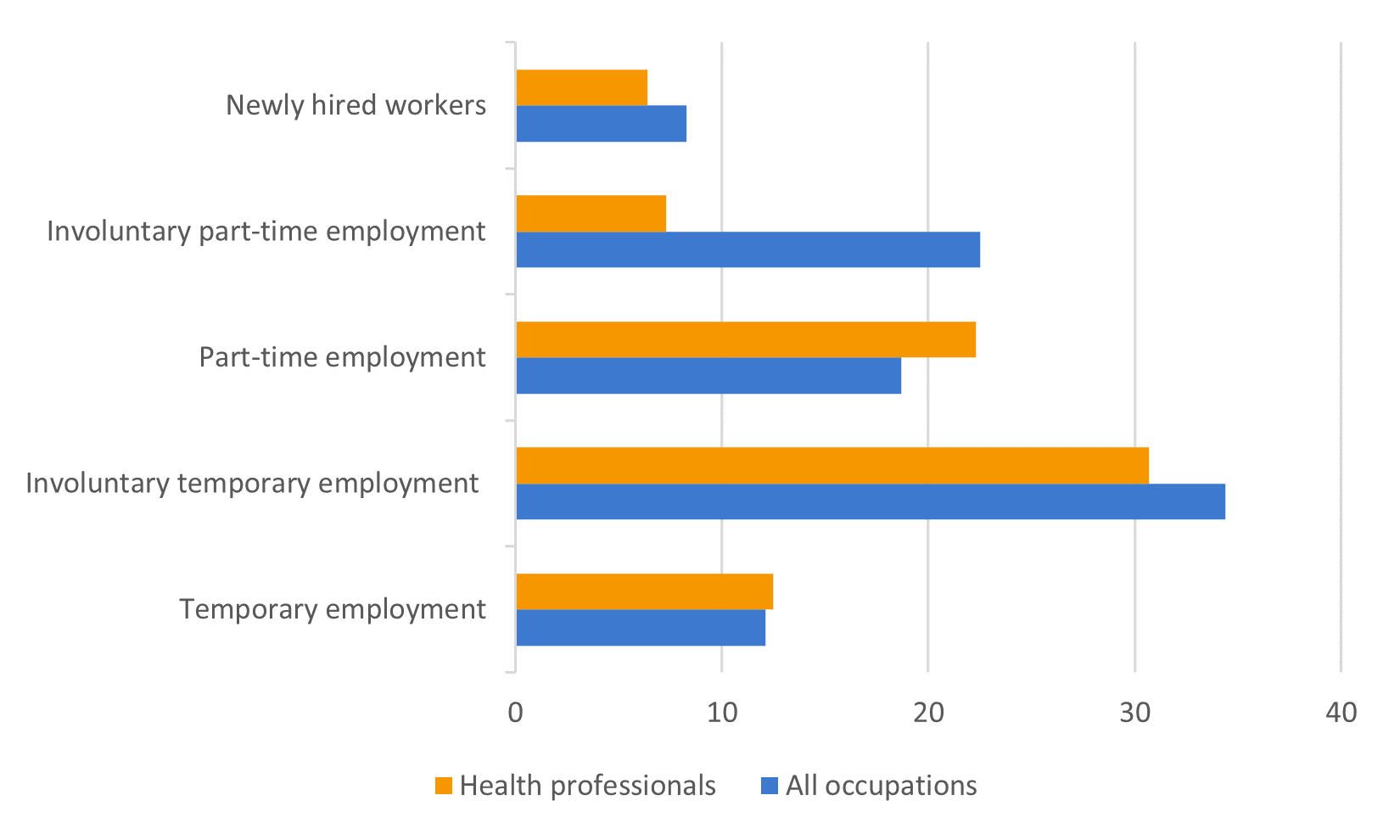
Source: European Labour Force Survey. Microdata. Own calculations.
Skill needs and future trends
As workers in the health sector, health professionals’ most pronounced skill needs are communication and caring. Also, health professionals report that manual tasks are an everyday part of their job – both in terms of lifting heavy loads and being exposed to hazardous environments.
While almost all health professionals need to use digital devices for work, the exposure to different digital technologies is slightly lower than all occupations average. They also report under average need for digital upskilling, and digital skills training. While ICT penetration in health care is considered to be a major trend, it does not seem to affect most workers significantly – yet.
Despite the difficulties and stresses associated with health professionals’ jobs, workers remain satisfied and motivated. High levels of job satisfaction are even more impressive when considering the survey has been taken during the Covid-19 pandemic – an extremely challenging, and also dangerous period in health professionals’ careers.
Figure 8: Skills, training needs and job perception of health professionals (in %)
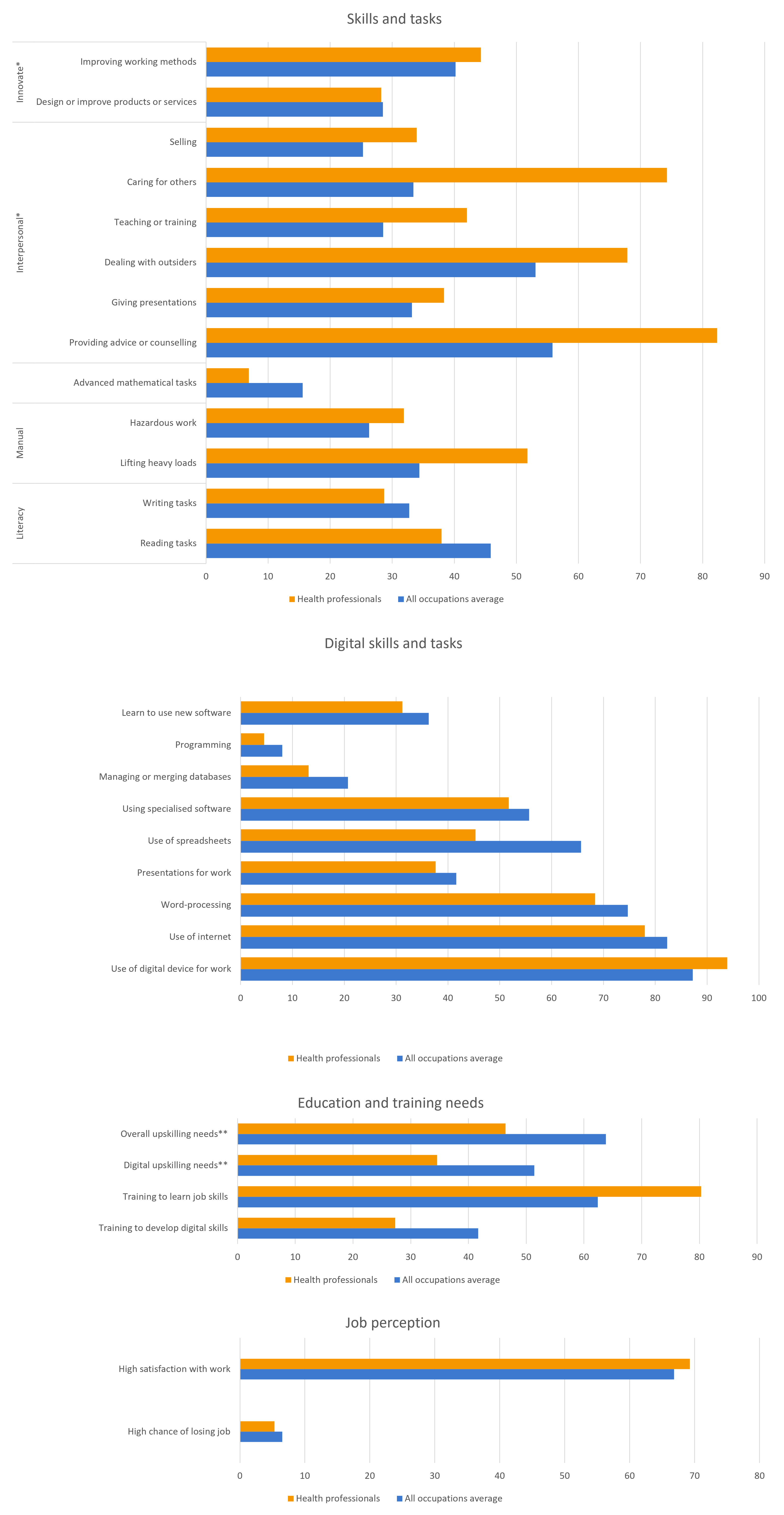
Source: European Skills and Jobs Survey. Microdata. Own calculations.
Unless stated otherwise, it is a share of people reporting that a task/skill is part of their job.
*Always or often
** Share of workers reporting these needs to a great or moderate extent.
Employment of health professionals is expected to increase quite much (by about 17 per cent) over the period 2022 to 2035. Employment in 18 countries grew at rates larger than 10 per cent in the past decade and it is forecast to do so in the next decade as well. The rest either remain stable or represent the opposite trend.
Figure 9: Past and expected future employment trends of health professionals
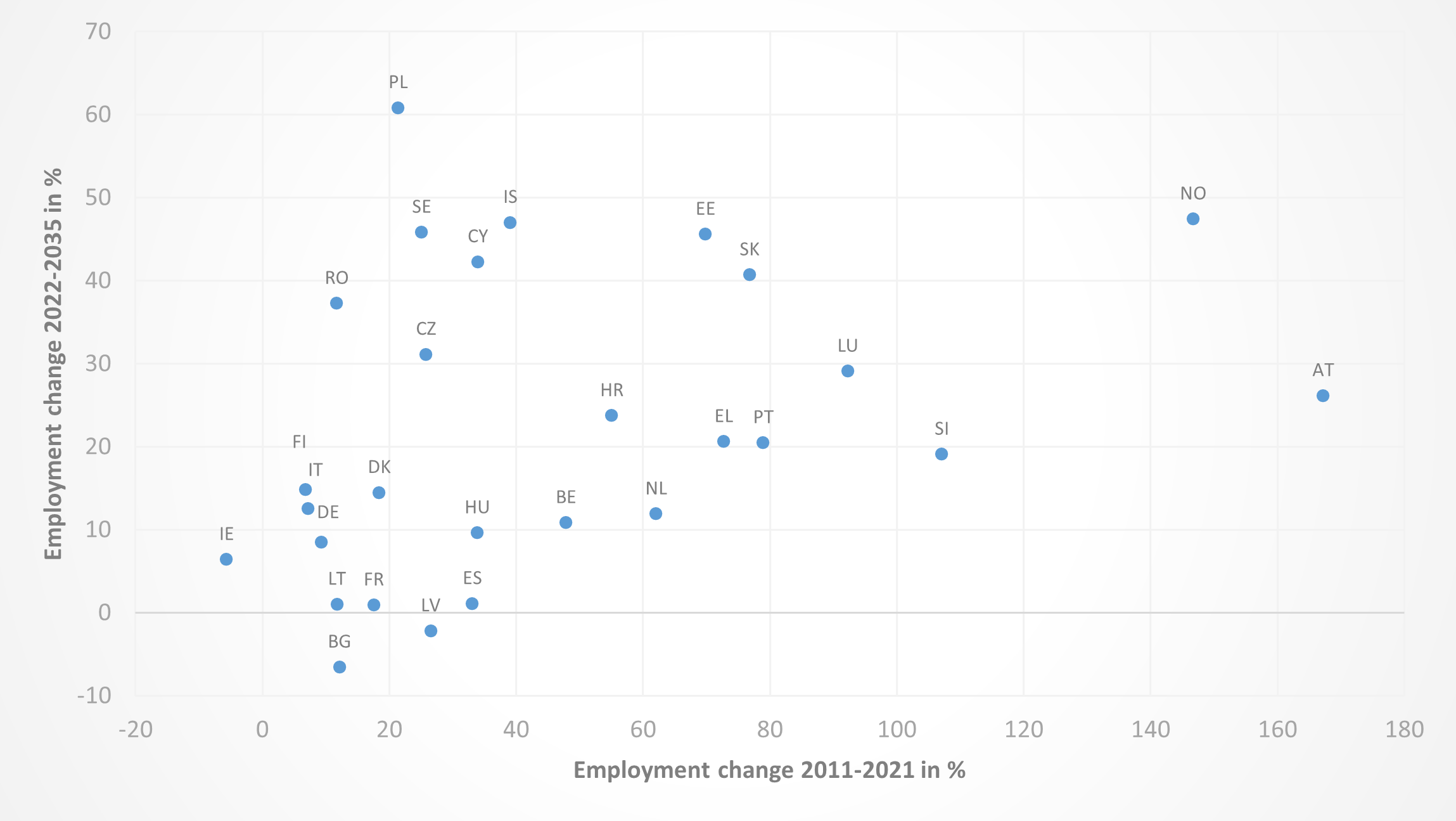
Source: European Labour Force Survey. Microdata. Cedefop Skills Forecast.
Note: Data for CY, EE, IS, LV and LU have lower reliability because of the small sample size.
LFS data for MT are not available.
Most job openings are a result of people leaving them for other opportunities, or those leaving the labour market completely (retirements; parent leave and such). This replacement demand is often much more substantial, and in the case of the health professionals it is estimated at 4.1 million workers, thus being more than four times as much as the new job creation. The rate of job openings – a comparison between all forecast job openings and current employment in the occupation – exceeds 50 per cent.
Figure 10: Future job openings for health professionals (000s)
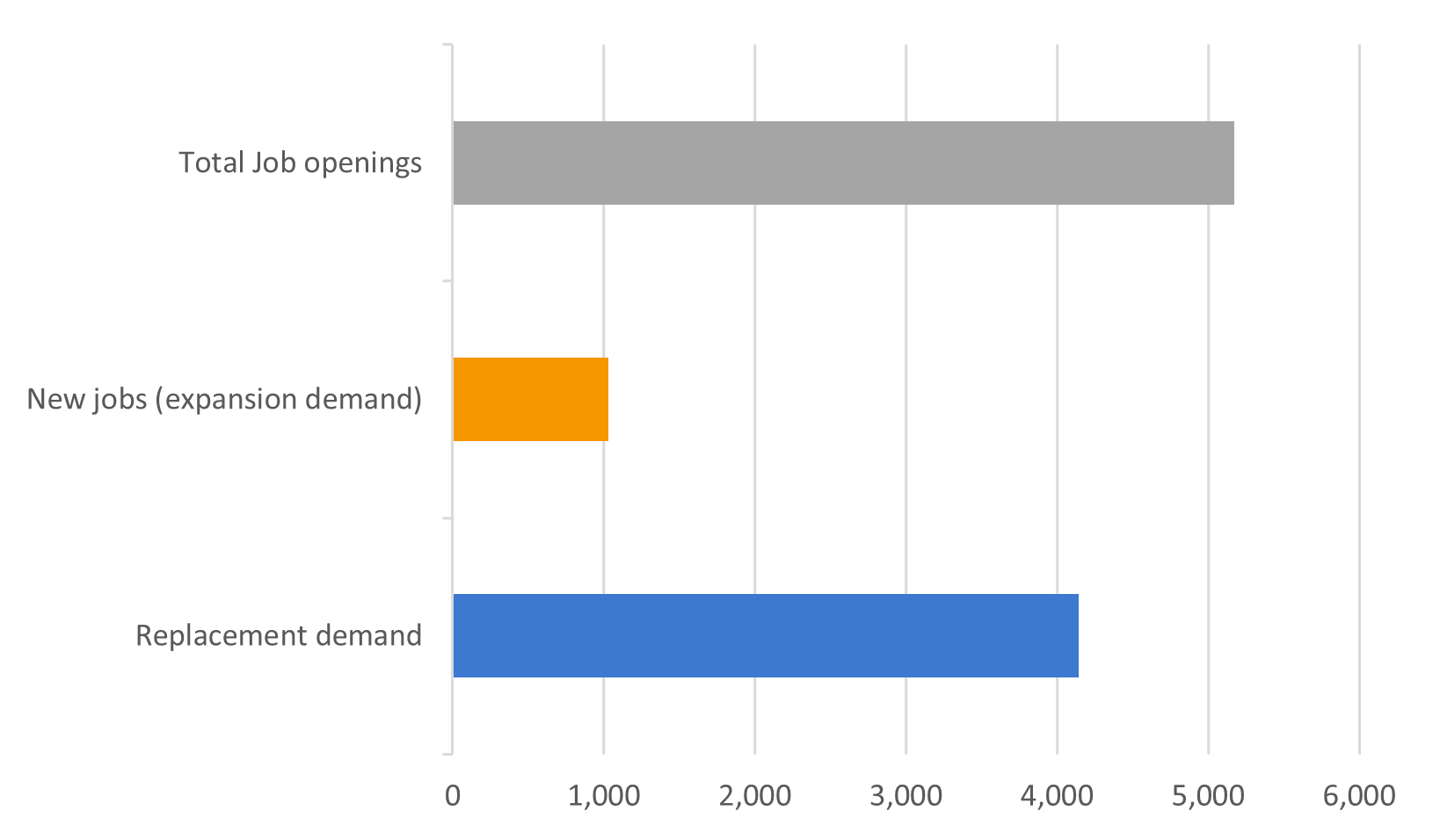
Source: Future job openings indicator based on the Cedefop Skills forecast. Own calculations.
Looking forward
Demographic trends like population ageing will shift the landscape of healthcare provision both in the content of care provision as well as in the volume of the healthcare demand. The changing sector is also challenged by digital and green transitions. A recent Cedefop (2023) report provides detailed information on the drivers of change in the care sector, in which health professionals - such as midwives and nurses - form a significant part (about 20%).
- Aging population in Europe is due to increase the need for healthcare professionals. The share of very old people (aged 80 or above) in the EU is projected to have a two and a half fold increase between 2021 and 2100 (Eurostat, 2022). This is set to raise much the demand for long-term care and services covering diseases typically affecting older people such as arthritis, mental health problems, and sensory impairment (Eurostat, 2019). Furthermore, it is expected that about half of the European population will develop cancer at some point in their life – another challenge for European healthcare. The Europe’s Beating Cancer Plan (2021) is the EU’s policy strategy, which seeks to counter cancer throughout its life course – by taking action in key areas like prevention, early detection, diagnosis and treatment, and improved quality of life for patients and survivors. The strategy foresees a greater integration of innovative technologies in patient-centred cancer prevention and care.
- Digital developments facilitate prevention and monitoring but create also skill needs. The Europe’s Digital Decade Policy Programme 2022 sets a target of 100% of EU’s citizens being able to access their electronic health records by 2030 (Decision (EU) 2022/2481). Access to clinical information through digitalisation and data sharing are key tools for the European healthcare systems. In 2022, the European Commission presented a proposal for a regulation on the European Health Data Space, which aims to streamline cross border information sharing related to health records. Apart from data sharing, digitalisation entails the adoption of new technologies and approaches to prevention, diagnostics, and treatment in personalised healthcare. Increased use of big data and AI are driving innovation in biotechnology and pharmaceuticals (Nature, 2022). Machine learning in artificial intelligence allows for more precision in diagnostics, developments of diseases and customised treatments (Secinaro et al, 2021). Also, digital diagnostics has potential to make healthcare more accessible in remote regions (Collingwood, 2021). While the new technologies offer a wide scope of application in healthcare, they also create new potential threats – such as data and privacy concerns, or automation bias (i.e. human doctors trusting more the judgment of the technology than their own). To avoid these scenarios, future healthcare professionals must also have awareness over the limitations of the algorithms that are used for automated diagnoses (Arora, 2020). The EIT platform provides detailed information on various technological innovations in healthcare in Europe. It connects healthcare providers with startups and entrepreneurs to address 21st century challenges from an interdisciplinary perspective.
- The healthcare sector will also be impacted by Sustainable Development Goals, which are linked to the European Green Deal. In the aftermath of the global Covid-19 pandemic, need for healthcare is projected to grow as extreme climate events and ecological deterioration continue to increase their intensity (Lancet Countdown Report, 2021). Health and well-being are affected by environmental determinants such as air and water quality, housing and urban environments, and noise pollution. The climate emergency makes many of these factors to play a detrimental effect on public health (EPHA, 2020). For example, the rise in greenhouse gas emissions increases a complex matrix of health impacts, including illness and injury related to extreme temperatures and weather events, spread of infectious diseases, water borne illnesses and air pollution. Extreme climate events like heatwaves are projected to increase in temperature, frequency, intensity and duration. In conjunction with demographic factors like older age and pre-existing medical conditions, this puts vulnerable groups at health risk. Changing European climate increases the incidence rate of vector-borne diseases, like dengue, yellow fever, West Nile fever as well as Lyme borreliosis and encephalitis.
- The treatment of medical waste – which was increased markedly during the pandemic- is important for the sustainability of healthcare systems (WHO, 2022). Healthcare professionals will need to upskill and expand their knowledge on waste management approaches to mitigate the environmental impact of the healthcare sector (Mokra & Loosova, 2021). This involves, among others, distinguishing between hazardous and non-hazardous waste, applying circularity principles (i.e. reuse, repair and repurpose products and taking special care of toxic substances (Health Care Without Harm Europe, 2020a). The sustainable transformation of the healthcare sector may also include bio-based or sustainable medications/medical products that use natural, renewable and sustainable resources across the value chain. Healthcare professionals may have to get better acquainted with plant-based medicines (Bilia & do Ceu Costa, 2021).
- Another challenge facing healthcare professionals in the coming years is the surge of multi-resistant bacteria, posing health risks to the public and people performing medical procedures. Antimicrobial resistance (AMR) is estimated to be responsible for around 33 thousand deaths in the EU annually, while also costing around 1.5 bn euros annually in healthcare costs and productivity losses.
- Covid-19 highlighted the weaknesses of public health systems and exposed health and safety issues for health professionals. At the same time the pandemic accelerated digitalisation of healthcare in Europe, for instance through data exchange and information sharing (Horgan et al, 2020). The combination of lockdown measures, increased workload and health risks amplified the volume and severity of mental health problems for healthcare professionals (e.g. stress, anxiety, depression and insomnia). As the risk of future outbreaks of global health crises remains, healthcare professionals will have to be equipped with sufficient methods and tools to take care of themselves and colleagues under prolonged periods of stress (Spoorthy et al, 2020).
A shortage of healthcare professionals potentially threatens the possibility to fill the projected number of job openings by 2035. A recent report by the European Labour Authority found shortages for some health professional jobs across several Member States. These include nursing professionals (which in 2021 constituted about 30% of health professionals workforce) as well as specialist medical practitioners. Both job profiles are cited as being in severe shortage.
Sustainable healthcare systems making the best use of available technology will require adequate levels of education as well as continuous professional training. Healthcare professionals will have typically completed between three and six years of higher education. Medical education may differ in content and structure between national education systems, but it is generally a highly regulated field of study. For example, becoming a Doctor of Medicine in Belgium (KU Leuven) means following basic medical training, which consists of bachelor’s and master’s degrees. In addition to that, residency training combined with an advanced master’s education is compulsory to become a practising physician. Similarly, the Medicine degree programme at the Medicine University of Vienna entails 12 compulsory semesters of study divided to three phases – the first lasting for two semesters, the second for six semesters, and the third four semesters. In the 11th semester, students take mandatory clinical training, working in a hospital environment under guided supervision.
In addition to accredited qualifications, healthcare professionals will be continuing professional education throughout their careers – to stay up to date with technological and scientific developments as well as strategic frameworks such as the green transition. Continuous training can be undertaken in many different formats and environments, like transnational projects or training courses.
Digitalisation is at the core of transformations unfolding in European healthcare in the years to come. In addition to being able to use digital technologies in patient care processes, healthcare professionals must also possess a degree of digital literacy for data management. Healthcare professionals in training can expect an increase in digital skills modules in their education programmes – these could include understanding the safeguards of data privacy, working with evidence derived from AI, and improved communication skills in telemedicine (EHP, 2021). An example of such continuous education is the DEN (Digital Education in Nursing) project, which aims to modernise the curricula of nursing studies by enhancing digital education. This entail developing digital pedagogical competencies of lecturers, sharing of best practices, and collaborations on various digital technologies. The project is a collaboration between nursing education providers in Sweden, North Macedonia, Serbia, Slovenia and Croatia.
As regards new types of diseases, the EU’s One Health Action Plan against AMR foresees further education of healthcare professionals on this topic to ensure adequate and proportionate response to the growing incidences.
Health education providers across Europe are increasingly collaborating in transnational projects aimed at forwarding the digital and green transitions in the sector. For example, the Healthcare Transformation Academy, co-managed by the European University Hospital Alliance and EIT Health, offers high-quality and affordable on-demand courses in innovation management, high-value care, digital transformation and leadership. For instance, under the Digital Health Transformation theme, these professionals can take certified courses in Digital Health Transformation in Health Institutions, Technologies for Digital Healthcare Transformation, Service Design for Digital Healthcare Transformation, and Implementing Digital Healthcare Transformation. The European Connected Health Alliance Group has recently launched a new website for healthcare professionals, where they can improve their digital skills and innovation readiness in clinical settings in the framework of the DISH project. Meanwhile, the PsychONskills project for nursing professionals combines skills development in the conjunction of digital competences and soft and psychological skills needed to work with cancer patients.
Healthcare professionals will also be able to improve their professional skills through lifelong learning modalities. Micro-credentials are short-term certified learning experiences which allow for personal and professional skills, knowledge and competence development on a specific theme. For example, the EuroTeQ Engineering University alliance offers a micro-credential in Essentials of Digital Health which gives an overview of the digitalisation in the health sector. Similarly, the Fraunhofer Academy offer online courses in Transformative Digital Skills for Healthcare, including modules in Machine Learning for Precision Medicine or Usability and User Experience (UX) of Medical Devices. In Ireland, Stericycle providers Healthcare Waste Management e-learning solutions to healthcare providers. Upon completion, participants will receive a certificate that they have passed modules on reviewing waste, healthcare risk waste segregation, waste storage, transport and treatment, and bio systems reusable sharps containers.
How to cite this publication:
Cedefop (2023). Health professionals: skills opportunities and challenges. Skills intelligence data insight.
Further reading
Arora, A. (2020). ‘Conceptualising Artificial Intelligence as a Digital Healthcare Innovation: An Introductory Review’. Medical Devices: Evidence and Research. Vol.13
Beręsewicz, M. and Pater, R. (2021). Inferring job vacancies from online job advertisements, Luxembourg: Publications Office, 2021. https://ec.europa.eu/eurostat/web/products-statistical-working-papers/-/ks-tc-20-008
Bilia, A. R. & do Ceu Costa, M. (2021). ‘Medicinal plants and their preparations in the European market: Why has the harmonization failed? The cases of St. John’s wort, valerian, ginkgo, ginseng and green tea’, in Phytomedicine. Vol. 81
Cedefop (2022). Microcredentials for labour market education and training. https://www.cedefop.europa.eu/en/publications/5587
Cedefop (2023). Skills in transition: the way to 2035. Luxembourg: Publications Office. http://data.europa.eu/doi/10.2801/438491
Collingwood, J. (2021). ‘Artificial Intelligence in Medical Diagnosis’. Southern Medical Association (SMA) published 7 October 2021.
Decision (EU) 2022/2481 establishing the Digital Decade Policy Programme 2030. Official Journal of the EU. L 323/4
European Commission (2019). The European Green Deal. COM(2019) 640 final
European Commission (2021). Europe’s Beating Cancer Plan. COM(2021) 44 final
European Commission (2022). Proposal for a regulation on the European Health Data Space. COM(2022) 197 final
EHP (European Health Parliament) (2021). ‘EHP7 Policy Recommendations: Digital Health Transition and Governance’, in European Health Parliament Seventh Edition.
European Public Health Alliance (EPHA) (2020). ‘A Healthy European Green Deal?’. Briefing.
Eurostat (2019). “Ageing Europe – 2019 edition”, Luxembourg: Publications Office of the EU,
Health Care Without Harm Europe (2020). ‘The European Green Deal: New opportunities for sustainable healthcare’. Blog post, published 29 June 2020
Health Care Without Harm Europe (2020a). ‘Sustainable healthcare waste management in the EU Circular Economy model’. Position paper, published November 2020
Horgan, D., Hackett, J., Westphalen, C.B., Kalra, D., Richer, E., Andreu, A.L, Lal, A.J., Bernini, C., Tumiene, B., Boccia, S., Montserrat, A. (2020). ‘Digitalisation and COVID-19: The Perfect Storm’, in Biomedicine Hub, Vol. 5, pp. 1-23
Lancet Countdown (2021). The 2021 report of the Lancet Countdown on health and climate change: code red for a healthy future. The Lancet, Vol. 398 (10311), pp. 1619-1662
Mokra, J. & Loosova, J. (2021). ‘Healthcare waste management processes and transition towards a circular economy’, in European Journal of Public Health, Vol. 31
Napierala, J.; Kvetan, V. and Branka, J. (2022). Assessing the representativeness of online job advertisements. Luxembourg: Publications Office. Cedefop working paper, No 17. http://data.europa.eu/doi/10.2801/807500
Secinaro, S., Calandra, D., Secinaro, A., Muthurangu, V., & Biancone, P. (2021). ‘The role of artificial intelligence in healthcare: a structured literature review’. In BMC Medical Informatics and Decision Making, Vol. 21
Spoorthy, M. S., Pratapa, S.K., & Mahant, S. (2020). ‘Mental health problems faced by healthcare workers due to the COVID-19 pandemic – A review’, in Asian Journal of Psychiatry, Vol. 51
WHO (2022). ‘Global analysis of health care waste in the context of COVID-19: status, impacts, and recommendations’. World Health Organization: Geneva
Data insights details
Table of contents
Page 1
SummaryPage 2
Employment and job demandPage 3
Skill needs and future trendsPage 4
Looking forwardPage 5
Further reading