You are here
- Home
- Publications and reports
- Data insights
- Care workers: skills opportunities and challenges (2023 update)
Care workers: skills opportunities and challenges (2023 update)
Summary
Health and social care is a crucial sector for the European economy, accounting for about 11 per cent of European GDP expenditure in 2020 (Eurostat). Care workers, who mainly work in the health and social care sector, account for around 3 per cent of all employment in the EU. These workers were at the forefront of coping with the recent Covid-19 pandemic. They are also central in the future design of health systems to cope with Europe’s ageing population.
Care workers are engaged with taking care and supervising children in various facilities, and with the personal care and assistance of patients and elderly, convalescent and disabled people in health care and residential settings. Jobs within this group include healthcare assistants, home-based personal care workers, childcare workers, and teachers’ aides.
For the latest analysis of the EU care sector, please read this Cedefop policy brief.
Key facts
- Around 6.2 million people were employed as care workers in 2022, which accounts for around 3 per cent of total EU employment.
- Between 2019 and 2020, during which the EU experienced economic lockdowns, 150 thousand care worker jobs were lost. Employment fully rebounded in the next years and by the end of 2022, it was 316 thousand workers above the pre-Covid-19 level.
- Most care workers – 68 per cent in 2021 - are employed in the health sector.
- Nearly two thirds of care workers (65 per cent) have attained a qualification level of ISCED 3 and 4 in 2021, equivalent to the education level achieved after completing upper secondary education. The qualification level of the occupation is not expected to change over the period to 2035.
- Care workers are mainly women. In 2021, only 12 per cent of care workers were men.
- The employment of care workers is projected to slightly increase between 2022 and 2035.
- By 2035 over 6.5 million people are projected to be working as care workers. This underestimates the true level of employment demand. An estimated 3.9 million people will be needed to replace those who are expected to leave the occupation - mainly as a result of retirement – in addition to the projected growth of an additional 373 thousand people. In other words, between 2022 and 2035 an estimated 4.3 million job openings will need to be filled.
- Population ageing making certain diseases more prevalent and technological change – including ‘gerontechnologies’ and digital health monitoring tools - will drive changes in the skills required of care workers in the future. Socio-economic developments prompting a decline in informal care will also affect future demand for care workers.
Employment and job demand
The employment of care workers has risen quicker in recent decade than in the case of similar occupations. The 2020 employment drop was only mild, and the recovery the year after was remarkably strong. Care workers are one of the highest shortage occupations in the EU economy and will likely remain one in the forthcoming decade.
Figure 1: Year-to-year employment change for personal care workers (2013-2022)
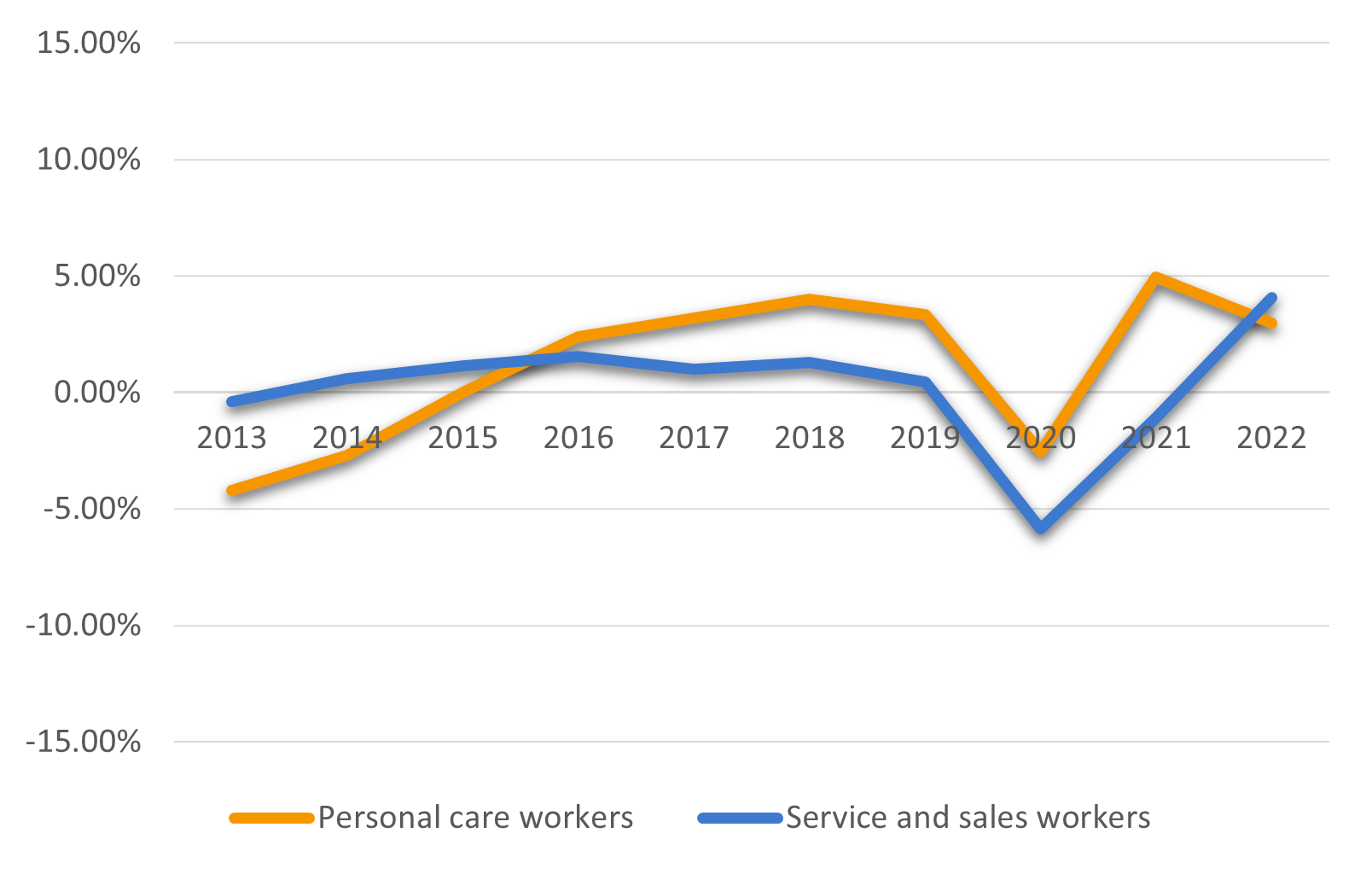 Source: European Labour Force Survey. Employed persons by detailed occupation (ISCO-08 two digit level) [LFSA_EGAI2D__custom_7778289]. Own calculations.
Source: European Labour Force Survey. Employed persons by detailed occupation (ISCO-08 two digit level) [LFSA_EGAI2D__custom_7778289]. Own calculations.
Around two thirds of care workers (67 per cent) are engaged as personal care workers in health services. People employed in these jobs are frequently occupied in health care and residential settings and provide personal care services and assistance to patients, convalescent and disabled people, and the elderly. Among other duties, they report to appropriate medical or social service workers; prepare patients for examination and treatment, and take part in planning the care of individuals.
About one third (32 per cent) of care workers are engaged as childcare workers and teachers’ aides. These provide care and supervision for children in various facilities such as schools, residential homes and childcare stations. Among other duties, they participate in teaching social skills to children and assisting them in preparing their education materials.
Over time the share of employment accounted for by these two occupations has remained more or less stable.
Figure 2: Employment in care worker jobs (in %)
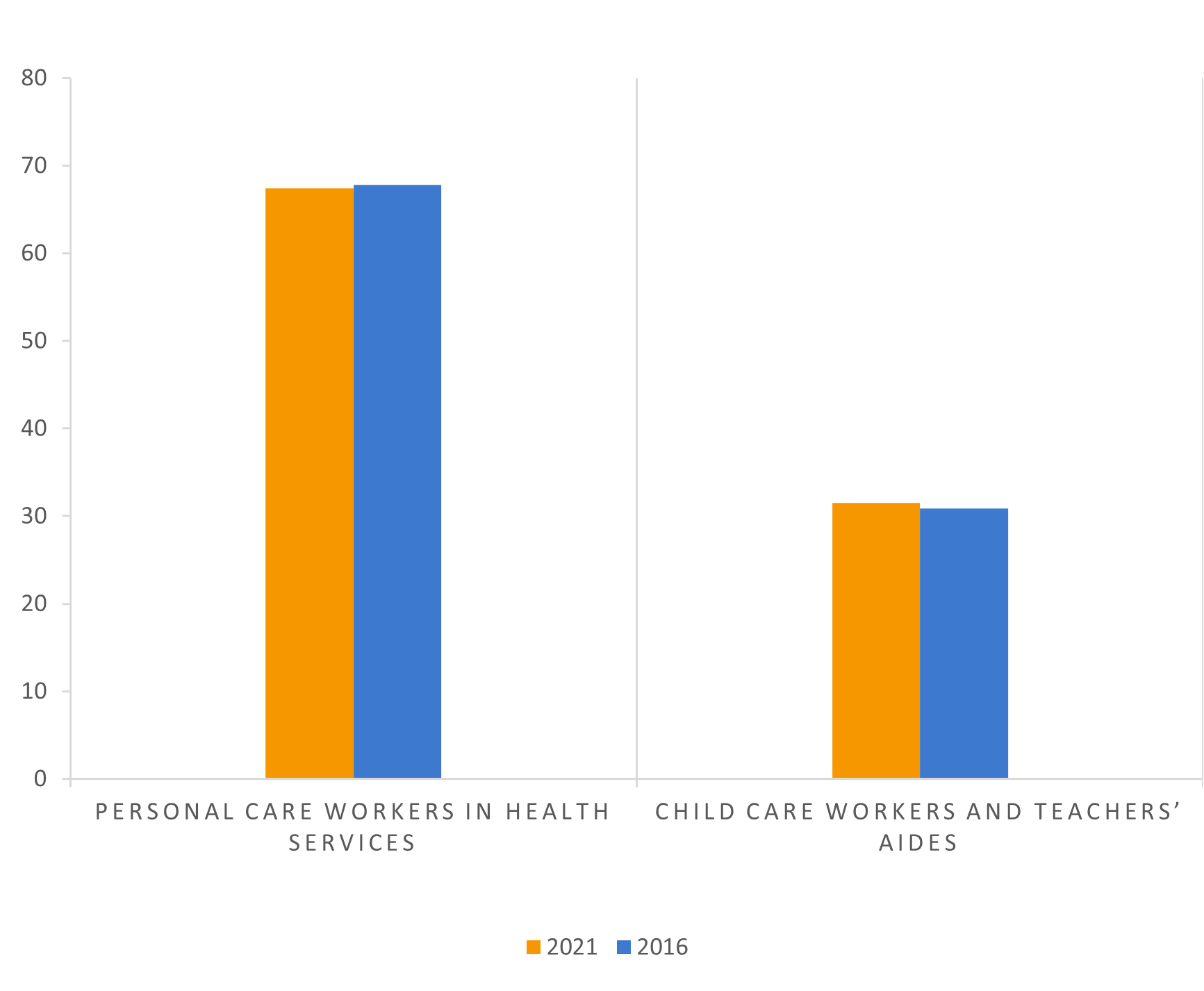 Source: European Labour Force Survey. Microdata. Own calculations.
Source: European Labour Force Survey. Microdata. Own calculations.
According to OJAs, demand for workers in health and care services is almost equally distributed. It is very likely many vacancies for personal care workers are not published online, because of high levels of undeclared work in home-based care. Therefore, the OJA-based analysis may obscure the true level of job demand.
For more details on skills demand and job openings for this occupation, please access the Cedefop’s Skills OVATE tool.
Figure 3: Online job advertisements for care workers (2022, in %)
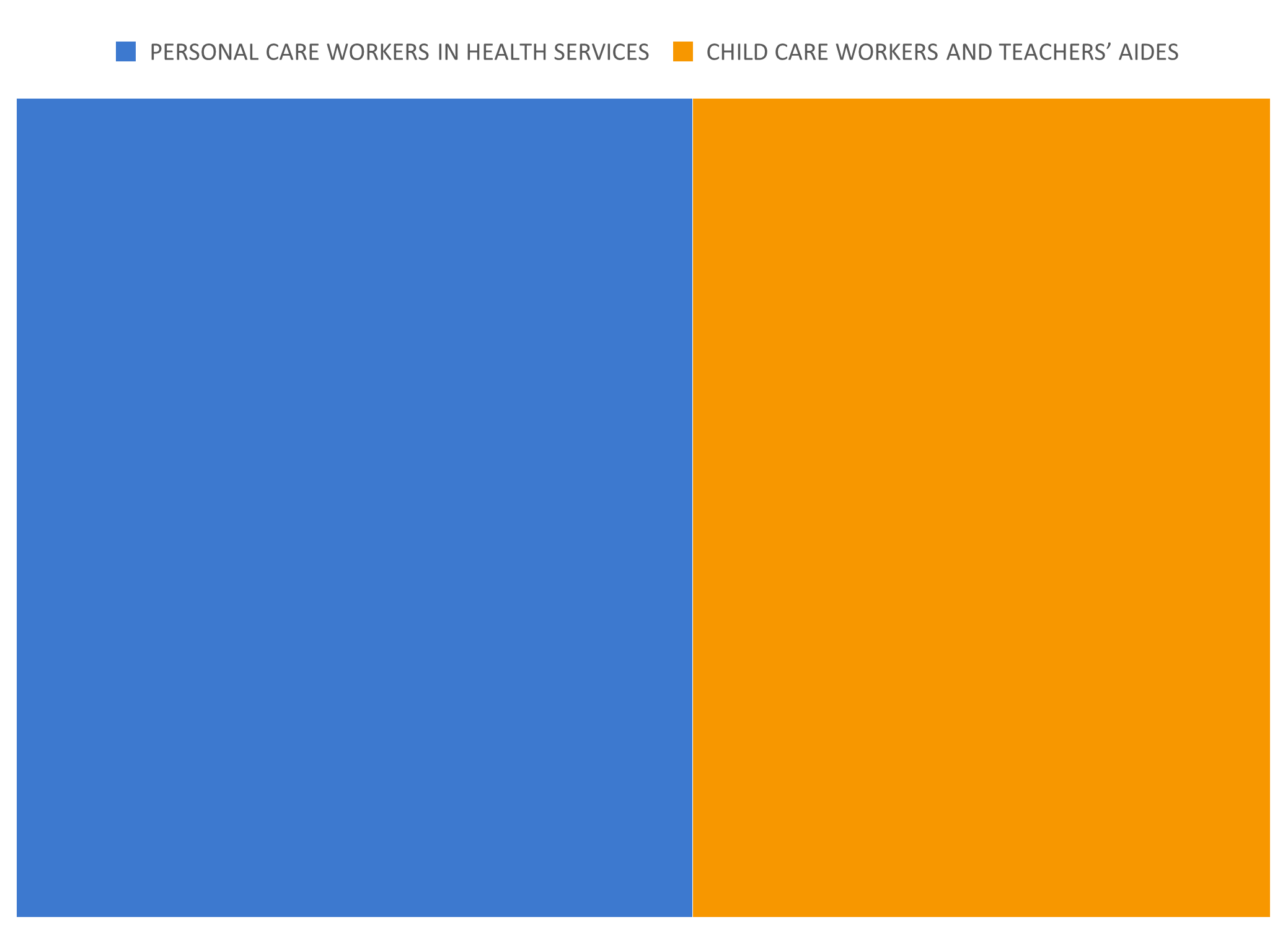 Source: Skills in Online Job Advertisements indicator based on Cedefop’s Skills OVATE. Own calculations. Note: Online job advertisements are by definition not equivalent to job vacancies. See Beręsewicz (2021) or Napierala et al. (2022).
Source: Skills in Online Job Advertisements indicator based on Cedefop’s Skills OVATE. Own calculations. Note: Online job advertisements are by definition not equivalent to job vacancies. See Beręsewicz (2021) or Napierala et al. (2022).
The health and social care sector employs the majority of care workers. In 2016, 72 per cent of care workers were employed in this sector. This had slightly declined in 2021 (see Figure 4). The arts, entrainment recreation, and other service activities and the education sector are the only other sectors with a significant number of care workers. Employment in the arts and recreation activities accounted for 13 per cent of care workers and remained unchanged in 2021, while employment in the education sector increased quite much over the period from 2016 to 2021, adding 222 thousand more care workers in the sector.
Figure 4: The top sectors employing care workers (in %)
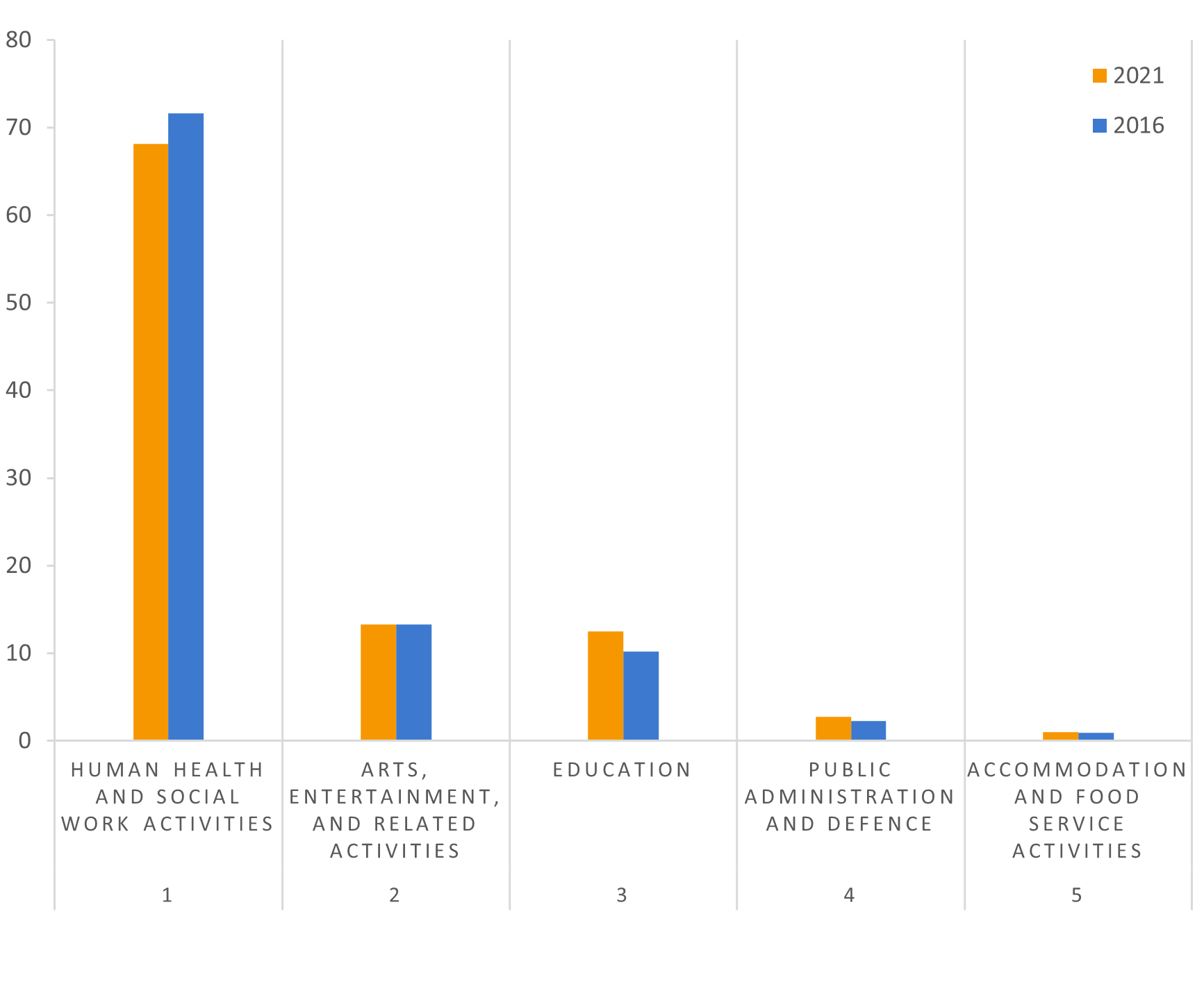 Source: European Labour Force Survey. Microdata. Own calculations.
Source: European Labour Force Survey. Microdata. Own calculations.
As regards the share of personal service workers within sectoral employment, these workers appear to be a significant part of the workforce in the health and social care, and household activities sectors. In 2021, they were the third largest occupation within the health sector (accounting for 19 per cent of its employment) and the second largest occupation within the household activities sector (consisting of 31 per cent of its employment).
The share of employment in each country varies significantly. Countries in the west and especially north of Europe employ much higher shares of care workers than countries in the south or east of Europe (Figure 5).
Figure 5: Care workers as a share of overall country employment (2021, in %)
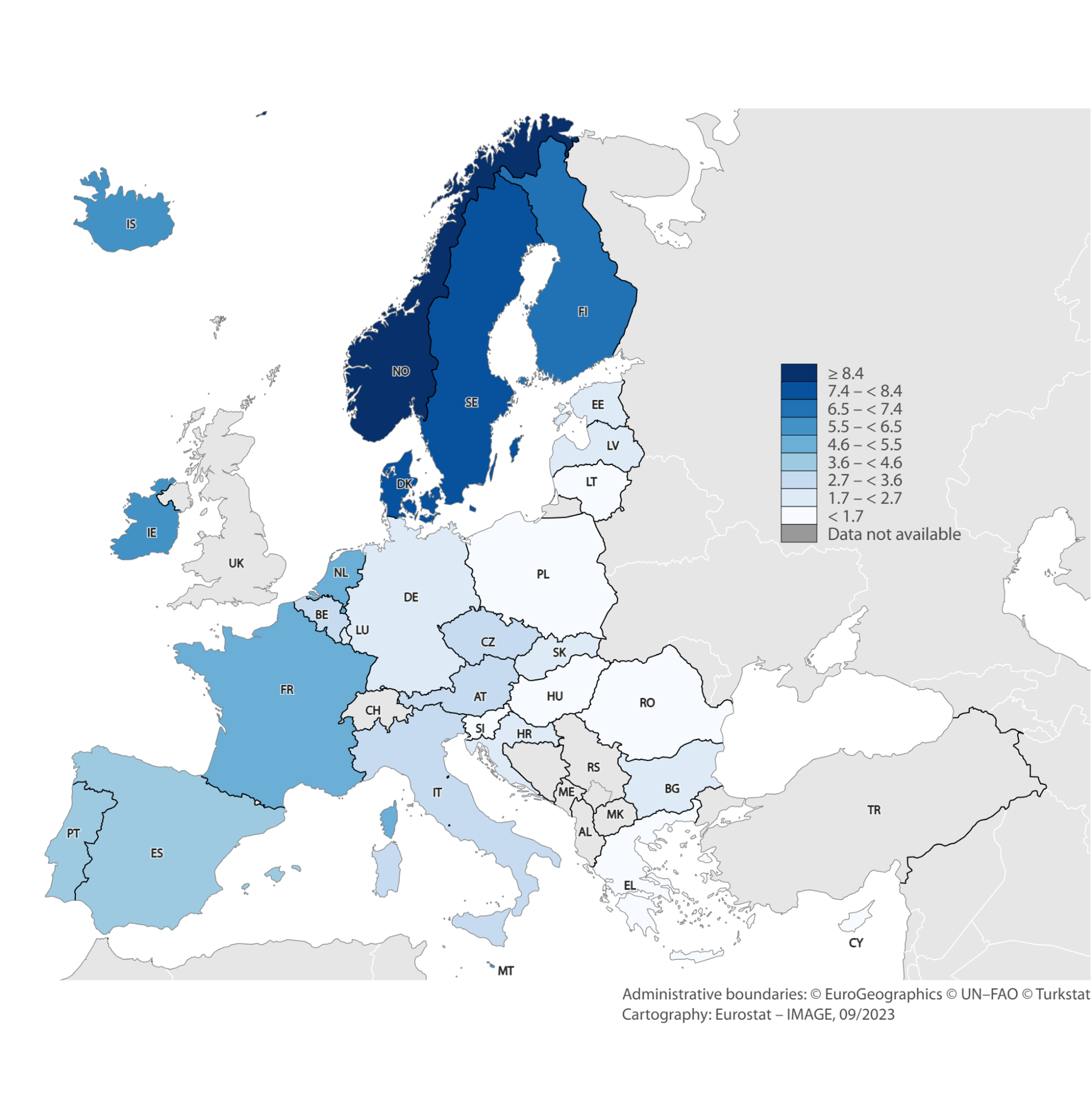 Source: European Labour Force Survey. Microdata. Own calculations. Note: Data for CY, EE, IS, LV and LU have lower reliability because of the small sample size. LFS data for MT are not available.
Source: European Labour Force Survey. Microdata. Own calculations. Note: Data for CY, EE, IS, LV and LU have lower reliability because of the small sample size. LFS data for MT are not available.
The workforce is comprised mainly of women. In 2021, male employment accounted for 12 per cent of employment, compared to 54 per cent across all occupations.
Care workers are a rather aged occupation compared to the average across all occupations (Figure 6). In 2021, 37 per cent of care workers were aged 50 to 64 years compared to 28 per cent across all occupations. Ageing and retirements of care workers will intensify the skills shortages in the occupation.
Figure 6: Care workforce by age (in %)
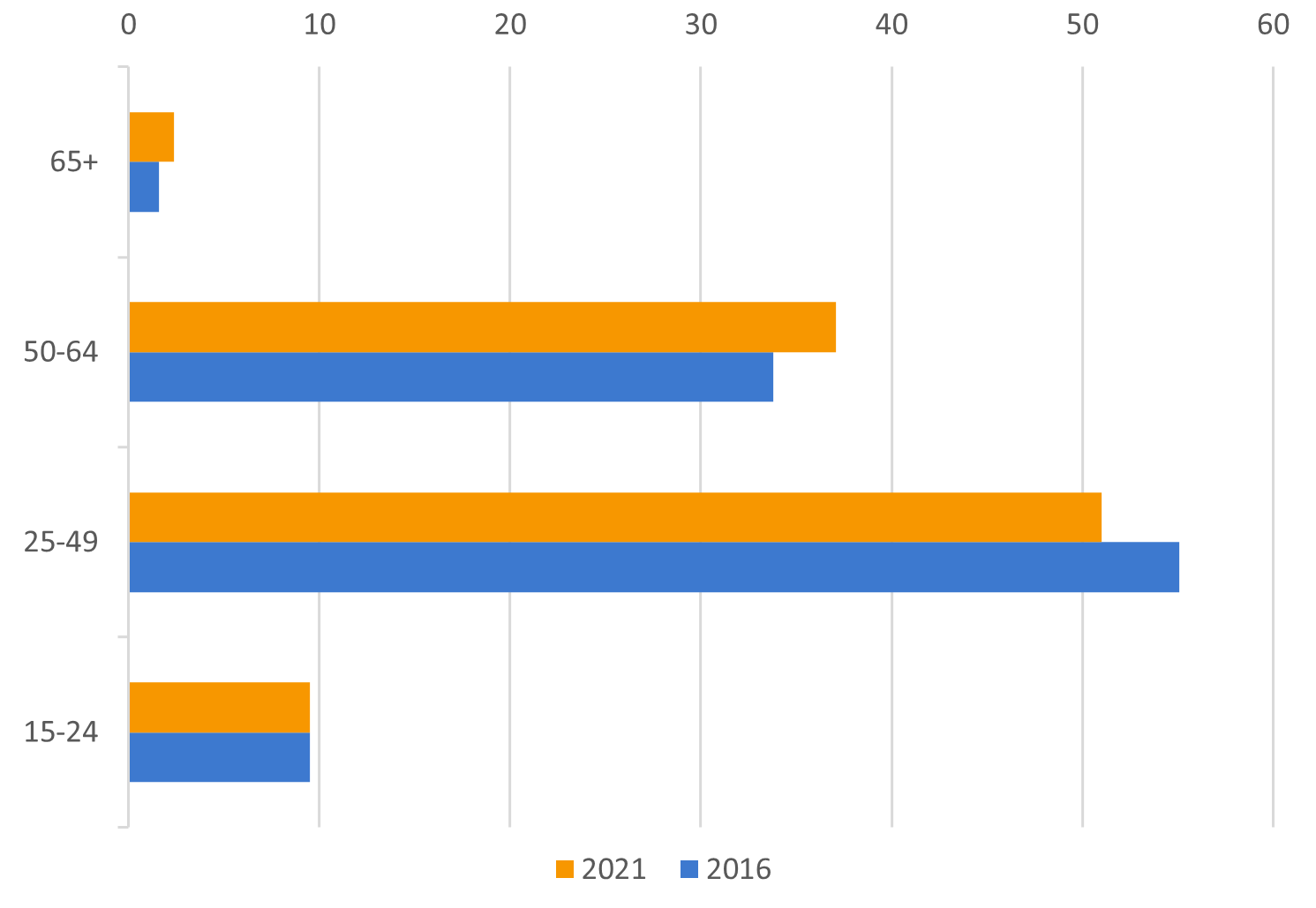 Source: European Labour Force Survey. Microdata. Own calculations.
Source: European Labour Force Survey. Microdata. Own calculations.
Care work is sometimes of a temporary nature. People may need care for a short period of time after an operation or injury. The need for home-based care may come to an end after a child grows up or a person passes away. To some extent, this is reflected in the percentage of workers employed on temporary contracts (see Figure 7).
Figure 7: Contract and hiring trends for care workers (in %)
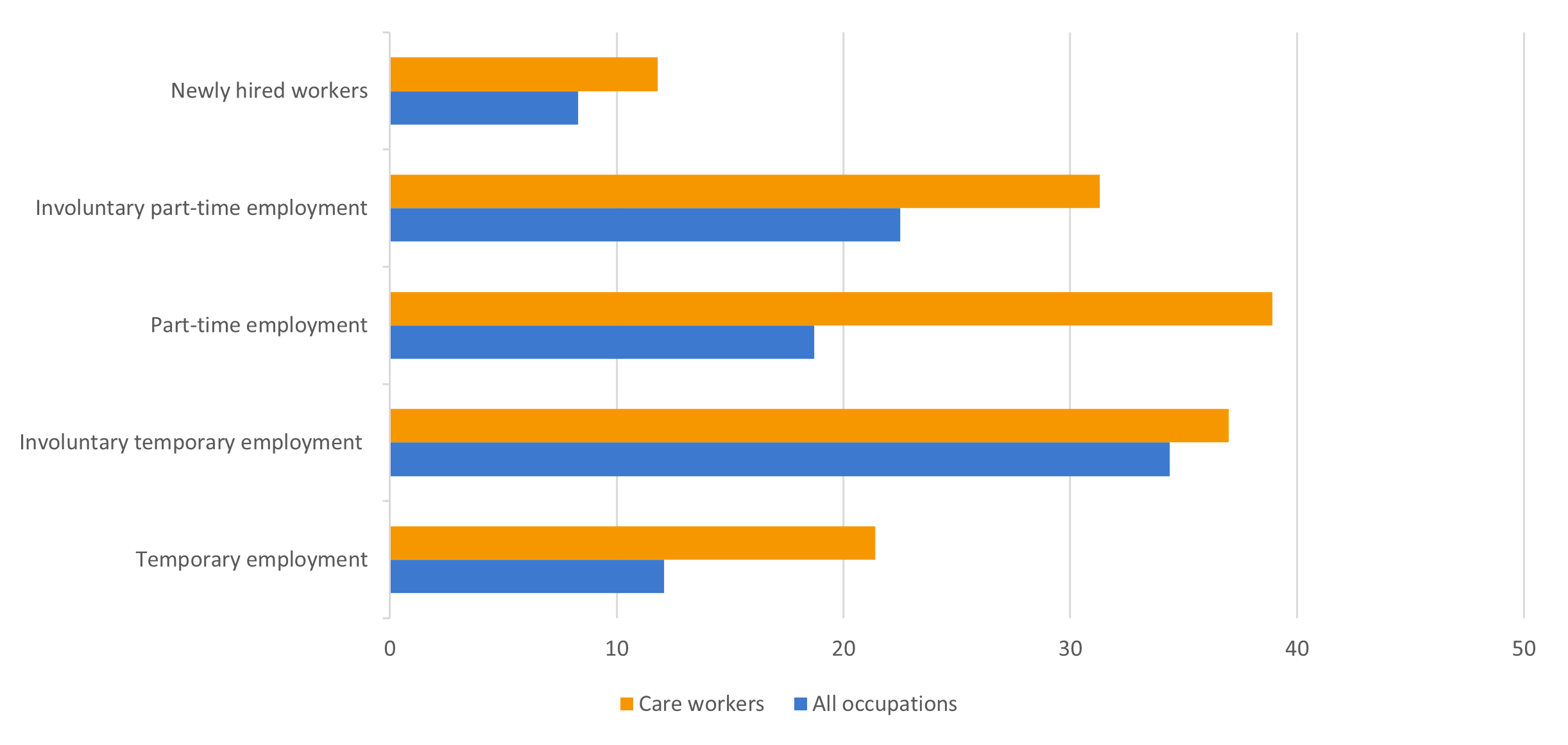 Source: European Labour Force Survey. Microdata. Own calculations.
Source: European Labour Force Survey. Microdata. Own calculations.
Skill needs and further trends
Since a majority of care workers are employed in the health sector, their interpersonal and manual tasks are of great importance. Caring for the disabled and elderly requires manual strength, and the care work is often stressful and even dangerous, like during the years of Covid-19 pandemic. Care workers work relatively little with digital technologies, although this is expected to change in future years. Care workers display remarkable job satisfaction, despite being a difficult and often low-paid occupation. The exact opposite is true for job security.
Figure 8: Skills, training needs and job perception of care workers (in %)
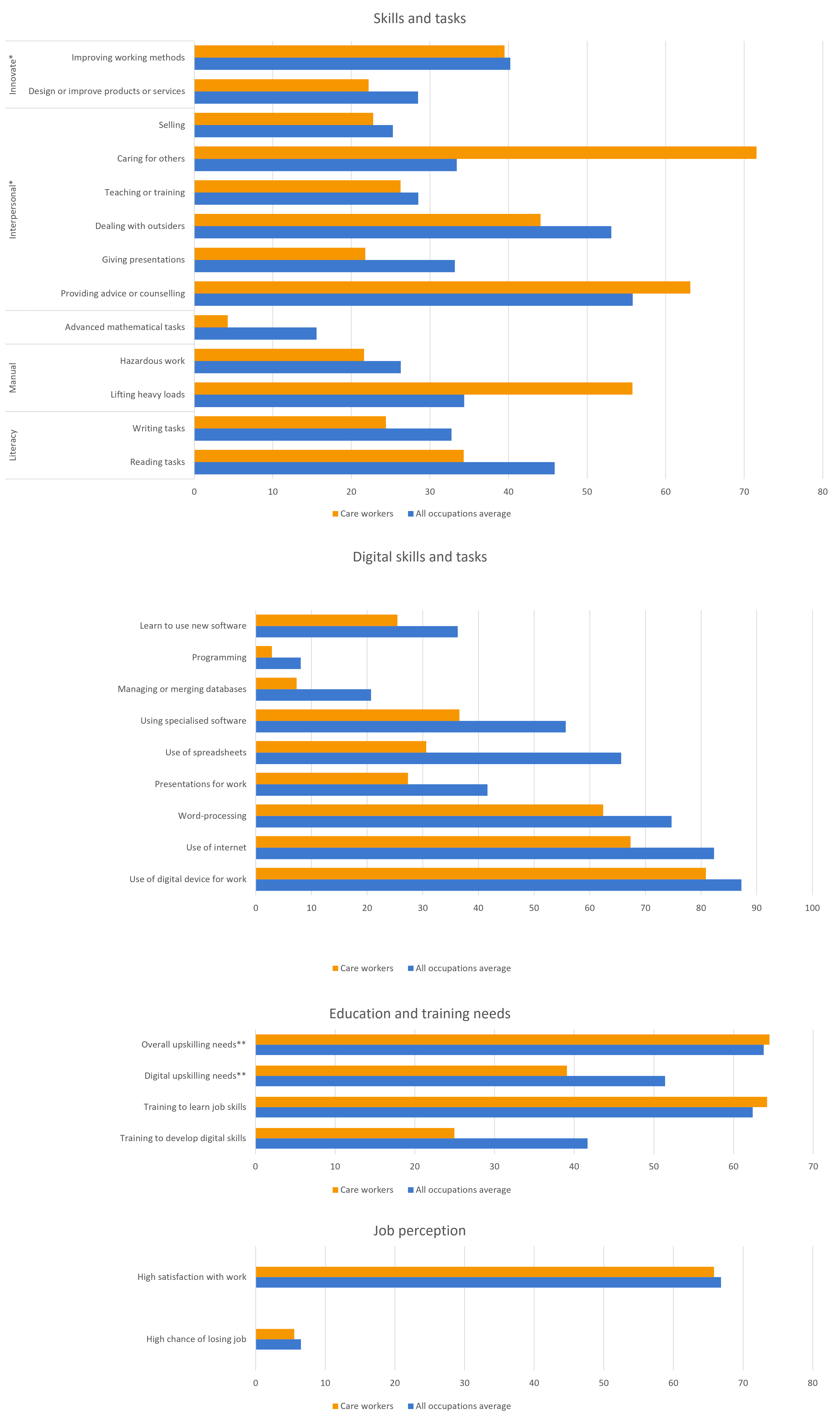 Source: European Skills and Jobs Survey. Microdata. Own calculations. Unless stated otherwise, it is a share of people reporting that a task/skill is part of their job.
Source: European Skills and Jobs Survey. Microdata. Own calculations. Unless stated otherwise, it is a share of people reporting that a task/skill is part of their job.
*Always or often
** Share of workers reporting these needs to a great or moderate extent.
Cedefop’s Skills forecast provides a detailed view of the future demand for care workers. Overall, employment for care workers is expected to increase twice as much as the overall employment over the period 2022 to 2035. This indicates that the upward trend in the occupation’s employment exhibited during the past decade will continue almost uninterrupted.
Future employment growth will be exhibited in most EU countries, albeit at varying rates. Figure 9 compares the employment growth experienced over the relatively recent past to that projected to take place in the future. Employment in most (21) countries grew in the past decade and it is forecast to do so in the next decade as well. Cyprus and Czechia are among those with the highest past and expected future growths, while especially France represents the opposite trend.
Figure 9: Past and expected future employment trend of care workers
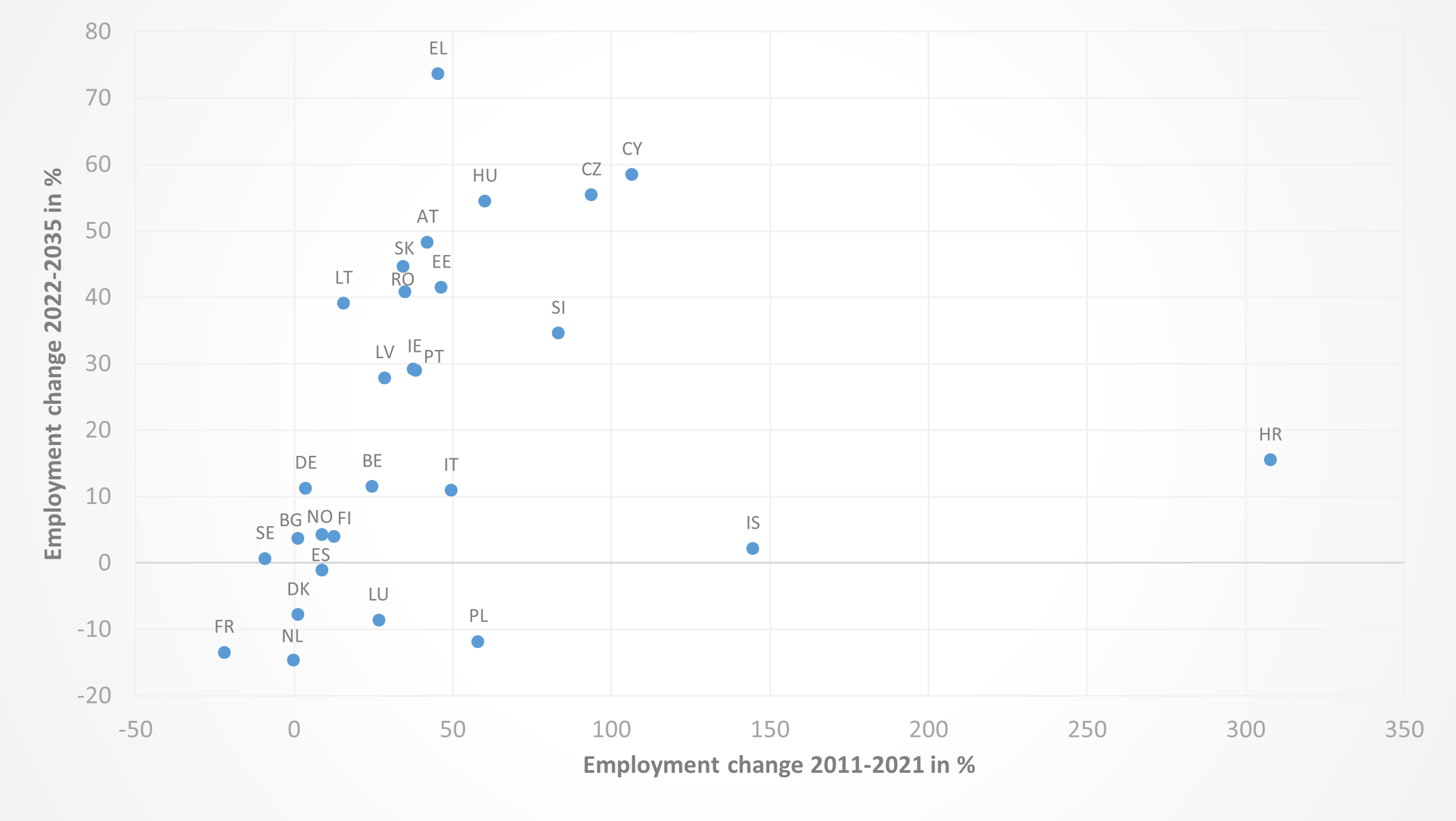 Source: European Labour Force Survey. Microdata. Cedefop Skills Forecast. Note: Data for CY, EE, IS, LV and LU have lower reliability because of the small sample size. LFS data for MT are not available.
Source: European Labour Force Survey. Microdata. Cedefop Skills Forecast. Note: Data for CY, EE, IS, LV and LU have lower reliability because of the small sample size. LFS data for MT are not available.
New job creation is, however, not the main driver behind job demand. Most job openings are a result of people leaving them for other opportunities, or those leaving the labour market completely (retirements; parent leave and such). This replacement demand is much more substantial, and in the case of the care workers it exceeds the new job creation more than tenfold, as it is estimated at 3.9 million (Figure 10). Meeting this future requirement may be challenging given the recently reported shortages of care workers and the rather poor working conditions for many of these workers (see below).
Overall, when expansion demand is added to replacement demand, an estimated 4.3 million job openings for care workers will need to be filled between 2022 and 2035.
Figure 10: Future job openings for care workers (000s)
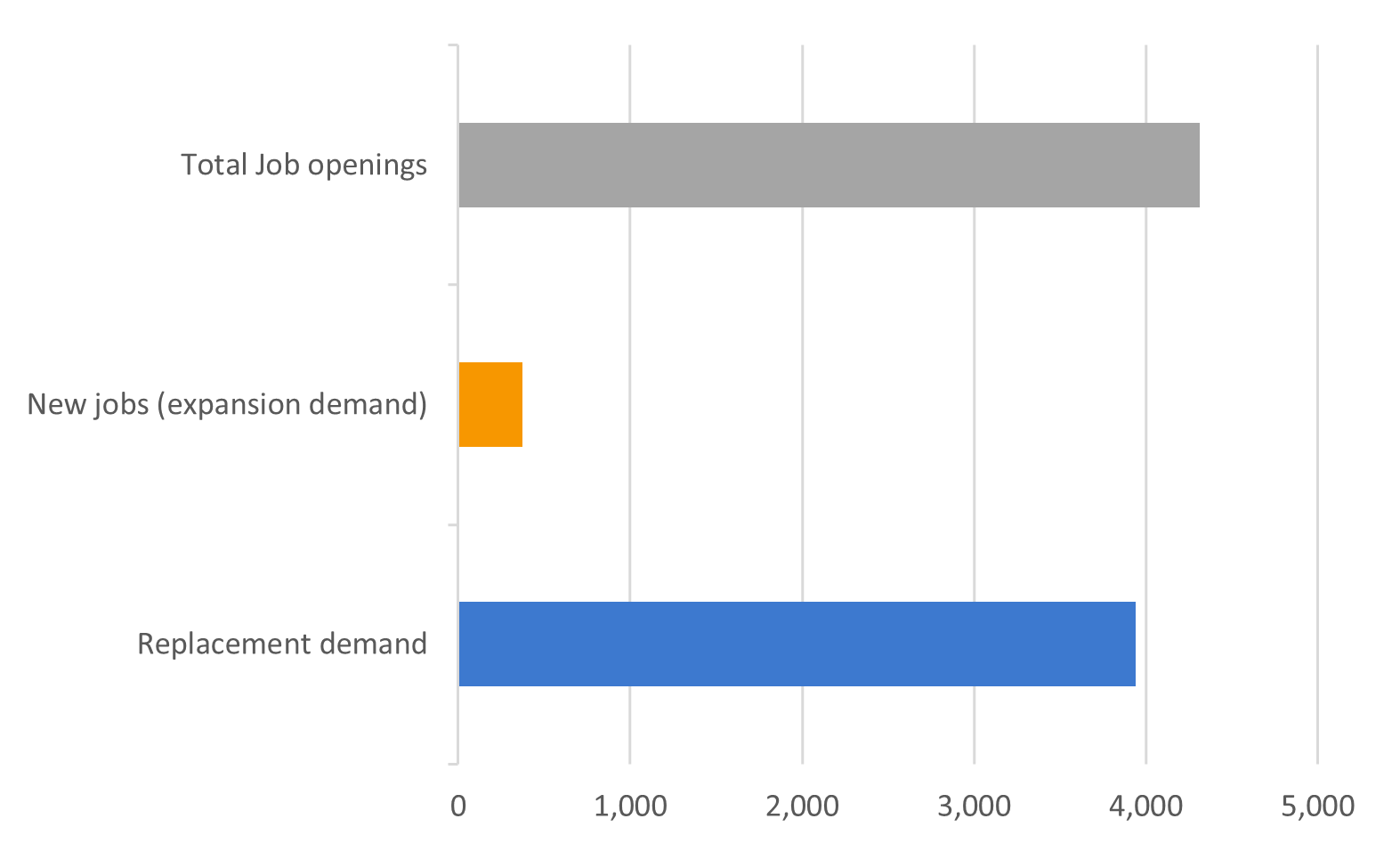
Source: Future job openings indicator based on the Cedefop Skills Forecast. Own calculations.
Nearly two thirds (65 per cent) of care workers held medium-level qualifications in 2021 (i.e. at ISCED levels 3 or 4). This is not projected to change much by 2035. However, the occupation is projected to undergo some upgrading in terms of qualifications. The share of workers with low levels of qualification (ISCED level 2 or lower) is projected to decline by 11 per cent while the share of highly qualified workers (i.e. those qualified at ISCED level 5 and over) is projected to increase by 9 per cent.
Looking forward
Factors driving the future skills needs of care workers relate much to the healthcare sector but are also affected by structural issues. European Commission in its long-term care report (European Commission, 2021) and Cedefop (2023) examined the evolving skill requirements for parts of the healthcare sector. Several key factors were identified that are likely to shape the future demand for care and the skillsets of care workers:
- Population ageing is foreseen to increase future need for healthcare services and personnel. Decreasing birth rates and higher life expectancy increases the numbers and population share of the elderly. According to Eurostat projections, the share of people aged 80+ years in 2100 will be 2.5 times more compared to its 2021 level (Eurostat, 2022). This prompts a marked increase in the demand for long-term care and services related to diseases that typically affect older people (arthritis, mental health/dementia, and sensory impairment) (Eurostat, 2019).
- Socioeconomic developments such as the growing female labour market participation, changing family structures and emigration create the need to replace informal with formal care. This will require a more a person-oriented approach to care provision, as care workers will tend to be more involved in co-ordination of home care with other services (OECD, 2020). Close interaction between care workers and care receivers requires effective communication to facilitate care provision.
- The increasing penetration of technology into healthcare through the so-called ‘gerontechnologies’ is, according to a recent Commission report, likely to improve access to high-quality affordable care services and aid independent living. It will however require care workers to undergo additional training. Digital devices have introduced new ways of communicating and monitoring care work. For example, digital communication tools enable some tasks to be carried out remotely, while digital health monitoring tools make some aspects of care work more precise (Schwiter & Steiner, 2020).
- Growth in digital care work platforms is likely to increase women’s labour market activity and has the potential to create better quality employment that combines flexibility, security, and social rights of care workers. Rise in care services supplied through platforms could help reduce unpaid care work. At the same time, platform work largely remains insecure and precarious (Rodriguez-Modrono et al, 2022). Care workers suppling services through platforms should develop a skillset that includes basic digital competences, coupled with personal soft skills related to management, entrepreneurship, and adaptability. These are important for managing freelance work, which is quite common in platforms.
- Covid-19 increased digital evolution in care work to a certain extent but has mostly exposed ongoing shortages and structural problems in the profession. In a recent report by the European Labour Authority, health care assistants were identified as a shortage occupation in 11 EU countries. Another report by the World Health Organisation notes that structural problems related to working conditions, low pay, dissatisfaction with work-life balance, understaffing, insufficient training, and weak trade union presence contribute to insufficient recruitment and low tenure among care workers. It also warns that the problem of replacement needs for care workers is set to grow at an increasing pace.
- Residential care facility closures during the pandemic have led to an increase in non-residential care employment (such as day-care services, home care) by about 6 per cent per cent, according to recent report of the FORESEE project. Non-residential, i.e., home-based care tends to be more human resource intensive and personalised and requires heavier investments in soft skills related to communication, (event and crisis) management, and problem-solving. It is also carried out extensively by women, who already comprise more than three quarters of care workforce. If the shift towards non-residential care is maintained post-pandemic, soft competences will need to be part of the skill toolkit of more and more care workers.
|
“Care work – both paid and unpaid – has been drastically impacted by COVID-19. Paid care workers in the health sector have faced increased work loads and heightened risk of infection, while many in the domestic sector have lost their livelihoods in the face of lockdowns and social distancing measures. The burden of unpaid care and domestic work, which already fell disproportionately on women before the pandemic, has increased dramatically during the pandemic, and data shows that women are continuing to shoulder an unequal portion. Working parents, and mothers in particular, have had to juggle paid work with full-time childcare in the wake of school and daycare closures. The burden of caring for sick family members and collecting fuel and water, among other tasks that tend to fall disproportionately on women, have also increased during COVID.“ Source: UN Women, 2022 |
- Foreign workers are over represented among care workforce, and the majority of them comes from non-EU countries (Eurofound, 2020). In 2021, 5.7 per cent of all non-EU citizens were employed as care workers (Eurostat). Also, many home-based long-term care workers in central European countries such as Austria, Germany and the Netherlands come from Eastern Europe (Eurofound, 2021). Thus, competences such as knowledge of a foreign language and the ability to understand different cultural backgrounds are a must-have skill in the ‘toolkits’ of many future care workers. The fact that many foreign workers in EU countries belong to vulnerable groups (low-qualified, low-paid) attenuates the need for additional training. Also, varying qualification standards and training for the care workforce across EU countries result in different workforce skill compositions (Cedefop, 2023) and a mismatch between the skills supplied by foreign-born care workers and those demanded in the country where they are employed.
Equipping care with updated and new skills is important for coping with the EU’s ageing population, establishing adequate care provision in a post-pandemic world, and making the best out of new technologies in care. For the care workforce, skills update will likely be a task for Vocational Education and Training, as most care workers typically enter the workforce with vocational qualification at ISCED levels 3 and 4. According to Cedefop in 2019 and 2020 68 per cent of care workers aged 15-34 reported possession of a vocational qualification.
With respect to IVET, current training policies for personal care workers vary across EU Member States, with some countries requiring vocational degrees and others not 9see the box below for an example of VET programme for care workers in Estonia). The same holds for employer obligations to provide additional training; only in a few countries such training is obligatory (Turlan, 2019). As the occupation’s skills mix becomes more technical, digital, and in general advanced, it is reasonable to assume that training requirements across the EU will increase, creating demand for VET provision. In addition, regulatory changes that establish cross-border qualification recognition can be a means for coping with existing mismatches between skills supply from foreign workers and skills demand in the country where they are employed.
|
Care worker (120 ECTS vocational training programme) The training programme of professional care workers takes two years to complete. By combining practical work experience with courses, the future care workers will be trained in different aspects of care work as well as the future developments in this occupation. By the end of the study programme, the care workers will be:
|
Meeting future skill needs requires also efforts to make sure that IVET proves to be attractive to would-be care workers. Recently reported shortages for care workers and the poor working conditions in the profession have recently activated policymakers in some EU countries. Their interventions concerned easing the recruitment process of care workers, provision of additional training, and improving working conditions (Cedefop, 2023).
Caring is an intensive task by nature that often (e.g., in home-based care) takes place on almost a 24/7 basis, leaving little time for long-term training. In such cases, the provision of short lifelong learning tools like micro-credentials can be an important means for enhancing the professional profiles of care workers with new skills. Micro-credentials are a fast-growing method of certified education. They certify the learning outcomes of short-term learning experiences such as courses or training. Flexible by nature, they offer a targeted approach to individuals for developing specific skills, competences and knowledge for professional and personal development. An example of short short-term certified training is provided in the box below:
|
Care-related training courses The German section of international Catholic relief, development and social service organisation offers a selection of courses and trainings related to care work. Ranging from legal, to social, medical and psychological topics, these courses include for example:
Source: Caritas Akademie, Germany |
The recently announced European Care Strategy can help care workers meet emerging skill needs. It is a means to aid EU Members States in creating a better working environment for care providers and combat staff shortages. It is the Commission’s response to the troubles brought about to care by the pandemic, and it aims to facilitate access to high-quality, affordable, and accessible long-term care and childcare services, and to address ongoing labour and skill shortages. The Strategy places great importance on high-quality standards and upskilling needs related to soft, digital skills and specialised technical knowledge (e.g., on diseases such as Alzheimer’s, chronic diseases, and diagnostics and treatment methods).
How to cite this publication:
Cedefop (2023). Care workers: skills opportunities and challenges. Skills intelligence data insight.
Further reading
Beręsewicz, M. and Pater, R. (2021). Inferring job vacancies from online job advertisements, Luxembourg: Publications Office, 2021. https://ec.europa.eu/eurostat/web/products-statistical-working-papers/-/ks-tc-20-008
Cedefop (2023). Handling change with care. Skills for the EU care sector. https://www.cedefop.europa.eu/en/publications/9185
Eurofound (2021). The pandemic aggravated labour shortages in some sectors; the problem is now emerging in others, blog article. July 21st, 2021.
Eurofound. (2020). Long-term care workforce: Employment and working conditions. Publications Office of the European Union: Luxembourg.
European Commission (2020). Renovation Wave: Doubling the Renovation Rate to Cu
European Commission (2021). Long-term care report: trends, challenges and opportunities in an ageing society. Volume I. Publications Office: Luxembourg.
European Commission (2022). Proposal for a COUNCIL RECOMMENDATION on access to affordable high-quality long-term care. COM(2022) 441 final.
European Institute for Gender Equality (2021). Gender inequalities in care and consequences for the labour market. Luxembourg: Publications Office of the EU.
European Labour Authority (2021). Report on labour shortages and surpluses.
Eurostat (2019). “Ageing Europe – 2019 edition”, Luxembourg: Publications Office of the EU,
Eurostat (2022). “Population structure and ageing”, February 2021.
FORESEE (2022).Impact of the Covid-19 pandemic on the social services sector and the role of social dialogue. FORESEE project report.
Napierala, J.; Kvetan, V. and Branka, J. (2022). Assessing the representativeness of online job advertisements. Luxembourg: Publications Office. Cedefop working paper, No 17. http://data.europa.eu/doi/10.2801/807500
OECD (2020). Who Cares? Attracting and Retaining Care Workers for the Elderly. OECD Health Policy Studies, OECD Publishing: Paris.
Rodriguez-Modrono, P., Pesole, A., & Lopez-Igual, P. (2022). Assessing gender inequality in digital labour platforms in Europe. Internet Policy Review, 11, 1-23.
Schwiter, K. & Steiner, J. (2020). Geographies of care work: The commodification of care, digital care futures and alternative caring visions. Geography Compass, 14, e12546.
Turlan, F. (2019). Social services workforce in Europe: State of play and challenges. Federation of European Social Employers report.
UN Women (2022). COVID-19: Rebuilding for Resilience: Care work.
World Health Organisation (2022). Health and care workforce in Europe: time to act. Copenhagen: WHO Regional Office for Europe.
Data insights details
Table of contents
Page 1
SummaryPage 2
Employment and job demandPage 3
Skill needs and further trendsPage 4
Looking forwardPage 5
Further reading